Is aggressive treatment of severe traumatic brain injury cost effective?
Researchers at the Perelman School of Medicine at the University of Pennsylvania have demonstrated that aggressive treatment of severe traumatic brain injury, which includes invasive monitoring of intracranial pressure (ICP) and decompressive craniectomy, produces better patient outcomes than less aggressive measures and is cost-effective in patients no matter their age––even in patients 80 years of age. These important findings can be found in the article "Is aggressive treatment of traumatic brain injury cost-effective? Clinical article," by Robert Whitmore and colleagues, published online March 6 in the Journal of Neurosurgery.
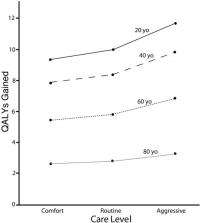
The authors set out to determine whether aggressive treatment of severe traumatic brain injury is cost-effective compared to less aggressive therapeutic approaches. "Severe traumatic brain injury" in this study is defined by a Glasgow Coma Scale score of 8 or less in which the motor component is 5 or less. These researchers created a decision–analysis model with which they could compare outcomes, costs, and cost-effectiveness of three treatment strategies: 1) comfort care consisting of one day in the intensive care unit followed by continued care in a medical-surgical unit; 2) routine care in which Brain Trauma Foundation guidelines were followed less than 50 percent of the time; and 3) aggressive management in which Brain Trauma Foundation guidelines were followed the majority of the time, with ICP monitored invasively and decompressive craniotomy performed. A review of the literature provided probabilities of Glasgow Outcome Scale scores (1 [death] through 5 [good outcome]) for each treatment group. The researchers took these Glasgow Outcome Scale scores and converted them into quality-adjusted life years in accordance with expectations of patient longevity and quality of life associated with the various Glasgow Outcome Scale scores. They also calculated estimates of direct costs (acute and long-term medical care) and indirect costs (loss of productivity) for patients 20, 40, 60, and 80 years old.
In every age group aggressive care resulted in better outcomes (more quality-adjusted years) than routine care, and routine care resulted in better outcomes than comfort care. (Comfort care was included in the analysis to broaden the comparison of outcomes and costs, but it is not suggested as a treatment choice.) In the case of an average 20-year-old patient, aggressive care produced 11.7 ± 1.6 quality-adjusted life years, whereas routine care only yielded 10.0 ± 1.5 quality-adjusted life years. The difference between these two numbers is highly significant (p < 0.0001). At older patient ages, the effectiveness of aggressive care was not as great as that in the 20-year-old patient, but it remained better than routine care at all ages. Aggressive care also proved to be less costly for most patients. Taking into account both direct and indirect costs, the researchers found that aggressive care was significantly less costly than routine care in the average 20-year-old patient ($1,264,000 ± $118,000 for aggressive care and $1,361,000 ± $107,000 for routine care). Aggressive care continued to be less costly until one looked at the 80-year-old patient, at which point it became more costly than routine care. To determine the cost-effectiveness of aggressive care in the average 80-year-old patient, the authors divided the difference in costs between aggressive care and routine care ($170,978 – $128,432 = $42,546) by the difference in effectiveness between these two groups (3.2758 – 2.7951 = 0.4807). They found that each quality-adjusted life year that is gained by implementing aggressive care, rather than routine care, costs society approximately $88,000. The authors point out that cost-effectiveness depends on the willingness of a society to pay for improved outcomes. Recent numbers posited have exceeded $100,000 for each quality-adjusted life year. Using that number as a threshold, the researchers found that aggressive care is the most cost-effective strategy for all age groups.
The authors point out that this is the first time that long-term societal benefits of aggressive treatment of traumatic brain injury have been demonstrated. Although initially aggressive treatment may appear more expensive than routine or comfort care, over time improvements in patient outcome shift the balance and aggressive treatment proves to be the most cost-effective of the three treatment paradigms. Comfort care, on the other hand, is related to poor outcomes and high costs. It should only be used after aggressive treatment has failed or tests show that it will fail.
Speaking of the study, Dr. Whitmore mentioned his initial surprise that "even for an 80-year-old patient, higher upfront costs of aggressive TBI [traumatic brain injury] management (surgery and invasive monitoring) would still be cost-effective when the benefits (outcomes) of aggressive treatment are factored in." He continued, "We hope that physicians will consider the results of this study when faced with the decision of how aggressive to be in the elderly TBI patient."
More information: Whitmore RG, Thawani JP, Grady S, Levine JM, Sanborn MR, Stein SC. Is aggressive treatment of traumatic brain injury cost-effective? Clinical article." Journal of Neurosurgery, published ahead of print March 6, 2012; DOI: 10.3171/2012.1.JNS11962