Researchers develop novel antibodies to diagnose and treat Alzheimer's disease
Under normal circumstances, the tau protein is a hard-working participant in memory and normal brain functioning. But as is becoming increasingly evident, in Alzheimer's disease and other neurodegenerative diseases, tau not only ceases to play a productive role in brain health, but actually undergoes a Jekyll-and-Hyde transformation to become a misshapen villain that destroys brain cells.
Now a novel antibody technology developed by a scientific team at Beth Israel Deaconess Medical Center (BIDMC) provides the first clear distinction between two tau isoforms – one healthy and one disease-causing – and demonstrates that only the disease-causing isoform is found in the neurons of Alzheimer's patients and is exhibited at a very early stage of disease. Described in the March 30, 2012 issue of the journal Cell, the findings raise the intriguing possibility that the development of antibodies and vaccines that target only the disease-causing tau isoform could be used to diagnose, treat and potentially even prevent Alzheimer's before the onset of debilitating symptoms.
"Since Alzheimer's disease takes at least a decade to develop, the major challenge to halt memory loss is to identify the initial period when the tau protein is transformed from 'good guy' to 'bad guy,'" explains co-senior author Kun Ping Lu, MD, PhD, an investigator in the Division of Hematology/Oncology at BIDMC and Professor of Medicine at Harvard Medical School (HMS). "By developing an innovative approach to making antibodies, we have uncovered a new strategy to specifically remove disease-causing tau, while leaving healthy tau intact to carry out its important responsibilities."
The most common form of dementia in older individuals, Alzheimer's disease currently affects 5.4 million Americans and 30 million people worldwide. As the baby-boom generation ages and life expectancy continues to grow, these numbers are expected to increase dramatically with some estimates projecting that by 2050 Alzheimer's will affect 120 million people worldwide at a cost of more than $1 trillion in the United States alone. There is currently no effective treatment for the disease.
In healthy brains, tau serves to both assemble and support microtubules, the "scaffolding systems" that give neurons their unique shape. As part of this normal function, phosphates are routinely added and removed from tau. Phosphates exist in one of two different shapes, or isoforms: The isoform known as trans is in a relaxed shape, while the isoform known as cis is in a twisted shape.
Scientists have known that abnormal phosphorylation of the tau protein is implicated in Alzheimer's disease and that an enzyme called Pin 1 (prolyl isomerase), originally discovered in 1995 by Lu together with Tony Hunter, PhD, of the Salk Institute for Biological Studies, protects against the onset of Alzheimer's in various experimental model systems.
In this new work, Lu and co-senior author Xiao Zhen Zhou, MD, an investigator in the Division of Hematology/Oncology at BIDMC and Assistant Professor of Medicine at HMS, hypothesized that when tau is phosphorylated during the normal aging process, it is in the twisted cis shape and that in healthy individuals, the Pin1 enzyme bends the phosphate back into the relaxed trans isoform. They further posited that when Pin1 is diminished or absent, the untwisting process is disrupted, causing tau to stay in its twisted cis shape –resulting in the development of Alzheimer's symptoms.
However, in order to test this hypothesis, the scientists first had to develop a tool that could visualize and specifically distinguish the two distinct isoform shapes. "We developed a group of small protein fragments that mimic the twisted and relaxed tau shapes as antigens in order to generate antibodies," explains Lu. This one-to-one recognition is similar to a lock and key, enabling the investigators to clearly spot and identify the two distinct phosphate isoforms.
Armed with this new tool, the scientists proceeded to investigate tissue samples from normal human brains and brains of Alzheimer's patients at various stages of disease.
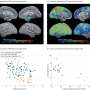
They discovered that although neither isoform is detected in normal healthy brain tissue, the twisted cis tau can be seen in humans with early dementia, also known as mild cognitive impairment. They further observed that as early dementia progresses to Alzheimer's disease, twisted cis tau accumulates only in diseased neurons at the locations that are known to affect memory and, in contrast, the relaxed trans shaped tau isoform does not appear.
Next, the Lu and Zhou team carried out a series of experiments to determine why these two different isoforms exhibited such distinct functions. "Our results consistently showed that the relaxed trans tau was able to assemble microtubules and was resistant to tangle formation, just like a native tau without any additional phosphate," explains Lu. In contrast, the situation with the twisted cis tau isoform was just the opposite, resulting in the loss of the protein's ability to assemble microtubules and leaving it prone to develop tangles and knots.
Finally, in a series of experiments in the test tube as well as in cell and animal models, the authors demonstrated that increasing Pin1 levels could prevent tau pathology, while reducing Pin1 levels resulted in tau knots and tangles.
"Ping Lu and his colleagues have developed a very clever strategy to generate specific antibodies against the two different isoforms of phosphorylated tau," says Tony Hunter, PhD, of the Salk Institute. "Their finding that only one of the two tau isoforms is prevalent in Alzheimer's disease tissue is an important advance and suggests that these new antibodies could be further developed into a therapy." In addition, he adds, the possibility of analyzing cerebrospinal fluid with these new antibodies holds great promise for diagnosing the onset of Alzheimer's disease and for predicting the severity of the disease.
"An immunization strategy that targets only the disease-causing twisted tau might enable diagnosis and treatment of memory loss at an early stage, when therapies are most likely to be effective," adds Lu, comparing the situation to that of hypertension.
"Early diagnosis of hypertension can lead to effective treatment to prevent complications," he notes. "But if high blood pressure goes undiagnosed, it can result in a stroke, at which point treatment is limited and extremely expensive. Similarly, early diagnosis of Alzheimer's patients before the onset of severe memory loss could offer doctors a much better chance of halting or even preventing this costly and devastating disease."