New drug prevents spread of human prostate cancer cells
A new drug developed by Northwestern Medicine scientists prevented human prostate cancer cells from spreading to other tissues without any toxic effects to normal cells or tissues. The drug turns off the "go" switch in the cancer cells and immobilizes them.
Prostate cancer is the second-leading cause of cancer death in North American males. Death is mainly caused by metastasis, prostate cancer cells moving out of prostate tissue and spreading to other organs.
"This is an extremely promising new therapeutic that locks down aggressive prostate cancer cells so they don't move," said Raymond Bergan, M.D., director of experimental therapeutics for the Robert H. Lurie Comprehensive Cancer Center of Northwestern University. "The spread of prostate cancer is what kills men. Cancer cells have a switch that tells them to keep moving all the time. This drug turns it off."
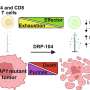
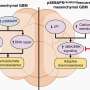
The drug works by binding to and disabling proteins in the cancer cell that instruct it to move, said Bergan, a professor of medicine at Northwestern's Feinberg School of Medicine and a physician at Northwestern Memorial Hospital.
The research was presented April 3 at the American Association for Cancer Research Annual Meeting 2012 in Chicago by Li Xu, a research assistant professor of medicine at the Feinberg School. She helped develop the drug, along with Karl Scheidt, an associate professor of chemistry at the Weinberg College of Arts and Sciences.
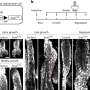
In the study, Northwestern researchers transplanted aggressive human prostate cancer cells into mice prostate tissue and fed the mice with the new drug for five weeks. The drug inhibited movement of the cells and prevented them from metastasizing to the lung, one of the tissues to which prostate cancer spreads in men.
Xu said she conducted extensive toxicity studies, including on normal human cells, and found that the drug, called KBU2046, is nontoxic and does not cause any harmful effects.
"We envision that this drug, if shown to be effective in clinical trials, could be used to treat men diagnosed with prostate cancer, so they wouldn't need more aggressive procedures," Bergan said. "Or, the drug could augment the effectiveness of surgery and radiation."
Bergan hopes to test the drug in a clinical trial.