Novel technology allows for noninvasive imaging of prostate cancer
Use of a novel, noninvasive imaging tool allowed researchers to measure free prostate-specific antigen in prostate cancer models and to visualize bone metastasis in a tumor-specific manner, according to results published in Cancer Discovery, a journal of the American Association for Cancer Research.
Results of this paper were presented here at an AACR Annual Meeting 2012 press conference on Saturday, March 31, 2012, at 4:00 p.m. CT in Room 20 A/B/C of the Hyatt Conference Center, adjacent to McCormick Place.
If further validated, the use of this tool, a prostate cancer-specific radiotracer, could potentially aid in treatment planning on an individualized patient basis, according to Michael J. Evans, Ph.D., research fellow in the Human Oncology and Pathogenesis Program at Memorial Sloan-Kettering Cancer Center in New York, N.Y., and colleagues.
A radiotracer is a small amount of a compound that has been “tagged” with a radionuclide. Patients are injected with the radiotracer, which aids in visualizing the tumor using positron emission tomography (PET).
In this study, Evans and colleagues examined the effects of 89Zr-5A10, the first radiotracer designed specifically to target free prostate-specific antigen (PSA), a known biomarker of prostate cancer that provides a more accurate measure of risk when compared with serum PSA.
“Once injected, the use of 89Zr-5A10 allows physicians to measure different biological properties among metastatic lesions within the same patient, which a serum biomarker cannot achieve,” Evans said.
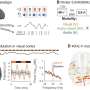
Researchers tested the utility of 89Zr-5A10 in a group of male mice with PSA-positive prostate cancer. The radiotracer localized to the tissue of castration-resistant prostate cancer, a state of the disease where serum PSA does not always reflect clinical outcomes, and sensitively measured declines in PSA expression induced by therapeutic intervention with the antiandrogen drug MDV3100.
The radiotracer also helped researchers identify metastatic bone lesions related to the primary prostate cancer. Traditional bone scans are unable to discriminate between malignant and nonmalignant lesions.
If translated to humans, this PET agent could help to stage prostate cancer, streamline the evaluation of prostate cancer therapies and aid in clinical trial management.
“The ultimate goal is to be able to predict the response of patients to new and existing therapies at an early stage, thereby personalizing their treatment and improving outcomes,” Evans said.
Given the success of this preclinical work, Evans and colleagues hope to translate the 89Zr-5A10 platform for a human trial by 2013.