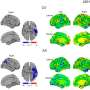
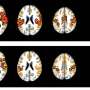
Examining adaptive abilities in children with prenatal alcohol exposure and/or ADHD
Prenatal exposure to alcohol often results in disruption to the brain's cognitive and behavioral domains, which include executive function (EF) and adaptive functioning. A study of these domains in children with heavy prenatal alcohol exposure (PAE), non-exposed children with attention-deficit/hyperactivity disorder (ADHD), and children without PAE or ADHD has found that, despite similarities in the relation between EF and adaptive abilities among children with ADHD or PAE, the patterns of abilities in these children were different.
Results will be published in the August 2012 issue of Alcoholism: Clinical & Experimental Research and are currently available at Early View.
"The comparison between populations with prenatal alcohol exposure (PAE) and attention-deficit/hyperactivity disorder (ADHD) is critical because children with PAE often have ADHD or symptoms of ADHD," said Sarah N. Mattson, associate director of the Center for Behavioral Teratology, professor in the department of Psychology at San Diego State University, and corresponding author for the study. "This comparison allows us to determine if deficits that are seen in children with PAE are specific to the disorder or are more generally associated with developmental conditions common in childhood. Clarifying which deficits are specific to PAE will pave the way for targeted interventions."
"This area of research is very practical because it focuses on trying to understand how important, complex thinking skills or EF relate to 'real world' behavior or adaptive functioning," said Heather Carmichael Olson, psychologist and faculty member of the department of psychiatry and behavioral sciences at the University of Washington.
Executive functions are a set of 'higher-order' thinking skills that can be thought of as the 'CEO' of the brain, Carmichael Olson explained. "These involve the ability to plan, organize, work toward goals, manage materials, and monitor oneself doing things," she said. "These also include the ability to stop impulses, control emotions, not make repeated mistakes, and be mentally flexible. Adaptive functioning refers to the wide variety of skills that people use to live day-to-day. While the specific skills change and become more complicated as children grow up, becoming teens and then adults, adaptive functioning skills always basically fall into three categories. These are communication, daily living skills, and socialization. The current study is especially relevant for individuals with ADHD, fetal alcohol spectrum disorders (FASD), or heavy PAE, who might have troubles in these two areas."
"Previous studies have shown that both EF and adaptive behavior are impaired in children with PAE," noted Mattson. "These impairments have been related to ADHD and the two disorders share some features. However, there are differences as well. Previous studies only looked at EF and adaptive behavior separately."
As part of a multisite study called The Collaborative Initiative on Fetal Alcohol Spectrum Disorders (CIFASD), Mattson and her colleagues examined three groups of children eight to 18 years of age: those with heavy PAE exposure (n=142), nonexposed children with ADHD (n=82), and typically developing "controls" (n=133) without PAE or ADHD. The children completed subtests of the Delis-Kaplan Executive Function System, and their primary caregivers completed the Vineland Adaptive Behavior Scales-II.
"The key finding of this study is that EF deficits predict adaptive behavior deficits in children with PAE," said Mattson. "This relation had been shown previously in ADHD, but this is the first study to confirm its existence in PAE. In addition, the relation between the two differed by group in that only nonverbal EF scores were predictive of adaptive behavior in the PAE group whereas the relation was more general in the ADHD group. The differential findings add further evidence to the argument that the pattern of deficits seen following PAE is unique. In other words, despite similarities in the predictive value of EF regarding poorer adaptive behavior among children with ADHD or PAE, the patterns of abilities in these children were different."
"There is much discussion in the fields of mental health and education about whether a diagnosis of FASD, or knowledge of heavy PAE, is at all useful in understanding a child's symptoms and coming up with treatment recommendations," said Carmichael Olson. "Some professionals have even wondered if the two clinical groups are really the same. But this study helps to show that the clinical populations of ADHD and FASD/heavy PAE are not identical, which is important in treatment planning. Only 60 percent of those with heavy PAE met criteria for ADHD. There was a different pattern of relationships between underlying thinking skills and 'real world' daily living skills for those with ADHD versus those with heavy PAE. And when a group of children had both heavy PAE and met criteria for ADHD, there was 'double trouble' and they had the most significant problems in daily life, and presumably greater treatment needs."
"Our findings add to the literature by comparing these two important childhood disorders," said Mattson. "By clarifying what is unique to FASD and what is shared with other developmental conditions, we can improve differential diagnosis and provide a framework for the development of targeted interventions."
Carmichael Olson agreed. "Although this article does not give specific treatment ideas, there are a few practical treatment ideas that might fit with study findings," she said. "For individuals with ADHD, having someone talk them through tasks might be helpful to improve success in daily living. Study results suggest this may not be as useful for those with heavy PAE. Instead, if individuals with heavy PAE have problems in non-verbal thinking which relates to success in daily life, it might be better to use a different style of learning supports. For instance, picture schedules that can show steps for daily life tasks for younger ages: pictures of the steps for getting dressed, loading the dishwasher, or even cleaning an apartment. Similarly, a smartphone 'app' that provides automatic reminders and visually walks an older individual with PAE through the steps of paying bills, or following a bus route, might be a low-cost intervention that would really help to improve daily function. As individuals with PAE grow older, they could learn to ask for help in coming up with these learning supports."