In the earliest stages of arthritis, high-impact exercise may worsen cartilage damage, study finds
Osteoarthritis, which affects at least 20 percent of adults in the United States, leads to deterioration of cartilage, the rubbery tissue that prevents bones from rubbing together. By studying the molecular properties of cartilage, MIT engineers have now discovered how the earliest stages of arthritis make the tissue more susceptible to damage from physical activities such as running or jumping.
The findings could help researchers develop tests to diagnose arthritis earlier in patients at high risk for the disease and also guide engineers in designing replacement cartilage. The results also suggest that athletes who suffer traumatic knee injuries, such as a torn anterior cruciate ligament (ACL)—which gives them a greater chance of developing arthritis later in life—should be cautious when returning to their sport following surgery.
"It's a clear signal to be careful of going right back out," says Alan Grodzinsky, an MIT professor of biological, electrical and mechanical engineering and senior author of a paper describing the findings in a recent issue of the Biophysical Journal. "Even though your knee may be stabilized, there's the possibility that deformation of cartilage at a high loading rate is still going to put it at risk."
Cartilage is packed with protein-sugar complexes known as aggrecans, each made of about 100 highly charged molecules called glycosaminoglycans (GAGs). Those molecules protect joints by absorbing water and causing the tissue to stiffen as pressure is applied.
"The cartilage is a stiff sponge, filled with fluid, and as we compress it, fluid has to percolate through these closely spaced GAG chains," Grodzinsky says. "The GAG chains provide resistance to flow, so the water can't get out of our cartilage instantly when we compress it. That pressurization at the nanoscale increases the stiffness of our cartilage to high-loading-rate activities."
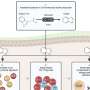
The MIT team set out to investigate how the molecular structure of GAG generates this stiffening over such a wide range of activity—from sitting and doing nothing to running or jumping at high speed. To do this, they developed a new, highly sensitive type of atomic force microscopy (AFM), allowing them to measure how aggrecan reacts at the nanoscale to very high loading rates (the speeds at which forces are applied).
Conventional AFM, which generates high-resolution images by "feeling" the surface of a sample with a tiny probe tip, can also be used to subject samples to cyclic loading to measure their nanomechanical properties. But conventional AFM can apply only up to about 300 hertz (cycles per second). Hadi Tavakoli Nia, the lead author of the paper, and Iman Soltani Bozchalooi, both graduate students in mechanical engineering, developed a modified system that can apply much higher frequencies—up to 10 kilohertz, frequencies relevant to impact loading of joints.
'A very floppy sponge'
Using this system, the researchers compared normal cartilage and cartilage treated with an enzyme that destroys GAG chains, mimicking the initial stages of osteoarthritis. In this early phase, collagen, which gives cartilage its structure, is usually still intact.
The researchers found that when exposed to very high loading rates—similar to what would be seen during running or jumping—normal cartilage was able to absorb fluid and stiffen normally. However, in the GAG-depleted tissue, fluid leaked out rapidly.
"That's what puts the collagen in trouble, because now this becomes a very floppy sponge, and if you load it at higher rates the collagen network can be damaged," Grodzinsky says. "At that point you begin an irreversible series of activities that can result in damage to the collagen and eventually osteoarthritis."
There is currently no good way to diagnose arthritis during those early stages, which are usually painfree. Many researchers are working to further improve magnetic resonance imaging (MRI) to test for loss of aggrecan, while others are looking for blood or urine markers. If such a test existed, it would be especially useful for monitoring patients who have experienced an acute knee injury. It is estimated that at least 12 percent of all osteoarthritis cases originated with a traumatic joint injury, Grodzinsky says.
Researchers in Grodzinsky's lab are now working to identify possible drugs that might halt the loss of aggrecan, as well as designing tissue scaffolds that could be implanted into patients who need cartilage-replacement surgery. The new AFM system should be useful for testing these scaffolds, to see if cells grown on the scaffold can produce the necessary tissue stiffening at high loading rates.
"These two aspects are really important: preventing cartilage degradation after injury and, if the cartilage is already damaged beyond its ability to be repaired, replacing it," Grodzinsky says.
Other authors of the paper are Yang Li, a graduate student in biological engineering; Lin Han, a former MIT postdoc; Han-Hwa Hung, a research specialist in biological engineering; Eliot Frank, a principal research engineer in biological engineering; Kamal Youcef-Toumi, a professor of mechanical engineering; and Christine Ortiz, a professor of materials science and engineering and MIT's dean for graduate education.
More information: www.cell.com/biophysj/abstract … 0006-3495(13)00277-4