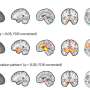
Stress test, brain scans pinpoint two distinct forms of Gulf War illness
Researchers at Georgetown University Medical Center say their new work suggests that Gulf War illness may have two distinct forms depending on which brain regions have atrophied. Their study of Gulf War veterans, published online today in PLOS ONE, may help explain why clinicians have consistently encountered veterans with different symptoms and complaints.
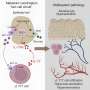
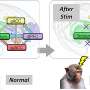
Using brain imaging that was acquired before and after exercise tests, the researchers studied the effects of physical stress on the veterans and controls. Following exercise, subgroups were evident. In 18 veterans, they found that pain levels increased after completion of the exercise stress tests exercised; fMRI scans in these participants showed loss of brain matter in adjacent regions associated with pain regulation.
During cognitive tasks, this group showed an increased use of the basal ganglia—a potential compensatory strategy the brain uses that is also seen in neurodegenerative disorders such as Alzheimer's disease. Following exercise, this group lost the ability to employ their basal ganglia, suggesting an adverse response to a physiological stressor.
In addition, "a separate group of 10 veterans had a very different clinical alteration," says lead author Rakib Rayhan, a researcher in the lab of the study's senior investigator, James Baraniuk, MD, a professor of medicine at GUMC.
In these 10 veterans, the researchers found substantial increases in heart rate. They also discovered that this subgroup had atrophy in the brain stem, which regulates heart rate. .
In addition, brain scans during a cognitive task performed prior to exercise showed increased compensatory use of the cerebellum, again a trait seen in neurodegenerative disorders. Like the other group, this cohort lost the ability to use this compensatory area after exercise.
Alterations in cognition, brain structure and exercise-induced symptoms found in the veterans were absent in the 10-participant matched control group, the researchers say.
"The use of other brain areas to compensate for a damaged area is seen in other disorders, such as Alzheimer's disease, which is why we believe our data show that these veterans are suffering from central nervous system dysfunction," Rayhan explains. He adds, however, that because such changes are similar to other neurodegenerative states, it doesn't mean that veterans will progress to Alzheimer's or other diseases.
These findings—a surprise to researchers—follow a study in Gulf War veterans published in March in PLOS ONE that reported abnormalities in the bundle of nerve fibers connecting the brain areas involved in the processing and perception of pain and fatigue.
Gulf War Illness is the mysterious malady believed to have affected more than 200,000 military personnel who served in the 1990-1991 Operation Desert Shield and Desert Storm.
Although veterans were exposed to nerve agents, pesticides and herbicides (among other toxic chemicals), no one has definitively linked any single exposure or underlying mechanism to Gulf War illness.
The symptoms of Gulf War illness—which have not been widely accepted by the public or medical professionals—range from mild to debilitating and can include widespread pain, fatigue and headache, as well as cognitive and gastrointestinal dysfunctions.
"Our findings help explain and validate what these veterans have long said about their illness," Rayhan says.
Gulf War veteran and study participant Carolyn Kroot, 54, a retired warrant officer in the Army National Guard, spent only six months in the Middle East during Operation Desert Storm. Just one week was spent in Iraq and Kuwait; the rest in Saudi Arabia. She believes she was exposed to sarin gas in Saudi Arabia. "Our chemical alarms were going off constantly," she says.
Within months of her return Kroot realized she was unable to focus on her work. "I had a hard time comprehending and remembering things, and I was always fatigued," she says. Her condition worsened, which prompted Kroot to constantly seek help. "I was always dismissed, and the favorite treatment was Motrin and an antidepressant. It was so frustrating.
"It has been liberating for me to have the validation, the confirmation, that there is indeed something physically wrong with me," Kroot says. "If I have brain damage, I am not upset. I have been living with this for decades, and the damage is done. I can't go back.
"At least I will have an answer," Kroot says. "I have been looking for one for much too long."