Rising rates of severe and fatal sepsis during labor and delivery
Rates of severe sepsis and deaths from sepsis among U.S. women hospitalized for delivery have risen sharply over the last decade, reports a study in the October issue of Anesthesia & Analgesia, official journal of the International Anesthesia Research Society (IARS).
"Maternal severe sepsis and sepsis-related deaths are increasing in the United States," concludes the report by Dr Melissa E. Bauer of University of Michigan Health System, Ann Arbor, and colleagues. Although the study identifies certain groups of women at increased risk, severe sepsis and death can occur during labor and delivery even in women with no recognized risk factors.
Rising Rates of Severe and Fatal Sepsis among Women in Labor
Using a national hospital database (the Nationwide Inpatient Sample), Dr Bauer and colleagues analyzed information on US hospitalizations for delivery from 1998 through 2008. Their goal was to identify trends in the frequency of maternal sepsis, including severe and fatal cases.
Sepsis is a serious medical condition in which the body has a system-wide inflammatory reaction to bacterial or other infections. In severe cases, sepsis can lead to multiple organ failure and death.
Extrapolated to the entire United States, the data represented approximately 45 million hospitalizations for delivery. Overall, sepsis occurred at a rate of 1 per every 3,333 women hospitalized for delivery. This rate did not change significantly over the 11-year period studied.
Severe sepsis occurred in about 1 out of 11,000 women. During the study period, the rate of severe sepsis approximately doubled: from about 1 in 15,400 to 1 in 7,250 women in labor.
Fatal sepsis occurred in about 1 out of 106,000 cases. Both severe and fatal sepsis increased by about 10 percent per year.
For Many Women with Severe Sepsis, No Known Risk Factors
The study identified several medical conditions associated with an increased risk of severe sepsis, including congestive heart failure, chronic liver and kidney disease, and lupus (systemic lupus erythematosus). Cerclage, or "cervical stitch"—a procedure performed to prevent premature birth—was also a significant risk factor.
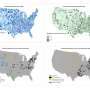
Other factors associated with an increased risk of severe sepsis were similar to those for other complications of labor and delivery, including older maternal age, African American race/ethnicity, and Medicaid insurance. However, none of these factors explained more than six percent of cases of sepsis during labor and delivery. Many women who developed severe or fatal sepsis had no known risk factors.
Sepsis is an increasing cause of complications and death among women in developed countries. Recent U.K. data have shown that deaths due to sepsis have nearly doubled over the past decade, "making sepsis the leading cause of direct maternal death in the United Kingdom," according to the authors.
The new study shows similar sharp increases in severe sepsis and sepsis-related deaths in the United States. The database study permits no conclusions as to what's causing the rise in severe sepsis among U.S. women. However, Dr Bauer and coauthors write, "This increase may have been due to similar factors as those identified in the United Kingdom… such as increasing microbial resistance, obesity, smoking, substance abuse, and poor general health."
The results also suggest that, while certain conditions increase the risk of severe and fatal sepsis, many cases occur in women with no recognized risk factors. That finding "underscores the need for developing systems of care that increase sensitivity for disease detection across the entire population," the researchers conclude.
More information: journals.lww.com/anesthesia-an … idity_During.24.aspx