New technique allows anti-breast cancer drugs to cross blood-brain barrier
Some breast cancer drugs can penetrate the blood-brain barrier (BBB), but they have not been very effective against brain metastases, whereas other, more effective anti-breast cancer drugs cannot penetrate the BBB at all. In a study published October 9 in the Journal of the National Cancer Institute, researchers used a new approach to selectively permeabilize the BBB at sites of brain metastases, even those 200 times smaller than currently detectable in the clinic.
To facilitate drug delivery to brain metastases, John Connell of the CRUK/MRC Gray Institute for Radiation Oncology and Biology, Churchill Hospital, Oxford, UK, and colleagues utilized the human pro-inflammatory cytokine, tumor necrosis factor (TNF), which they had previously shown could disrupt the BBB in rat brains.
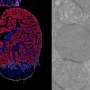
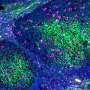
The researchers first verified the expression of TNF receptors in mouse as well as human brain metastases by immunohistochemistry. They then induced brain metastases in mice by injection of mouse breast carcinoma cells labeled with green fluorescent protein. After metastases were detected by MRI, the researchers injected the mice with TNF or its analog, lymphotoxin (LT) and 2-24 hours later, the radiolabeled anti-breast cancer drug, trastuzumab.
Radiolabeled trastuzumab was detected at the cerebral metastases in mouse brains that had been treated with TNF, whereas the drug was excluded from metastases in control mice treated with saline solution. The same effect was observed in brain metastases of mice injected with human breast cancer cells. Importantly, BBB permeability lasted long enough to allow delivery of the drug, peaking at 6 hours and lasting 24 hours.
The authors conclude that the work represents "…a novel approach to facilitating the delivery of therapeutic and diagnostic agents to cerebral metastases by exploiting a previously unknown phenotype of the vasculature of brain metastases." Connell et al. note, however, that although TNF was effective in mice, variability in TNF receptors in humans could have different effects and that this new technique must be validated in clinical trials.
More information: jnci.oxfordjournals.org/conten … jnci.djt276.abstract