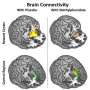
Inside the brains of addicts
Eating a good meal, a compliment on a new outfit, your team winning the football game – all these things make you feel good, and that's thanks to your brain's reward system.
Our brain's reward system evolved to respond to food and sex, activities we need to do to survive and pass on our genes. This "pleasure circuit" is driven by dopamine, a brain-chemical (or neurotransmitter) released from the brainstem and absorbed deep in the forebrain.
Unfortunately, this pleasure circuit can be hijacked by less healthy habits: whiskey drinking, smoking, binge eating, gambling, taking cocaine or heroin. Alcohol, nicotine, cocaine and heroin all buzz the brain the same way food and sex do – by activating dopamine.
Scientists are working to understand how addictive substances interact with these reward pathways with the goal of developing treatments to reverse damage or to block the buzz an addict gets from his or her drug of choice.
Virginia Commonwealth University researchers are hoping to develop medicines for treating drug addiction that may block ill effects of the dopamine system, particularly the depression of the reward circuit caused by addictive drugs.
"I think addiction treatment is moving in the direction of acceptance that addictions have a brain basis – that they are not just a disorder of choice or a moral failing," said F. Gerard Moeller, M.D., division chair of addiction psychiatry in the VCU School of Medicine. Moeller came to VCU from the University of Texas Health Science Center at Houston earlier this year.
"One of the advantages of being a physician scientist is a lot of what we do is driven by our experience with patients," Moeller said. "Addictions are more like a diabetes or hypertension model—a chronic disorder that we have treatments for controlling but not a cure."
At VCU, Moeller leads the Institute for Drug and Alcohol Studies (IDAS), which oversees a functional MRI research facility and plays a key role shaping the overarching vision of addiction medicine at VCU by fostering the link between clinical research and ongoing preclinical and genetic addiction research currently taking place at VCU. Researchers here are working to understand the neural differences that influence addiction, and the impact drugs have on the brain.
On the inside
Moeller's research uses brain-imaging technology to visualize how drugs change the brain and to find medications to treat addiction. Moeller has been an investigator funded by the National Institute on Drug Abuse, conducting clinical research on addictions since 1996. He has published work in more than 130 peer-reviewed publications in his research field.
Cocaine addiction is Moeller's main focus, though he also has studied MDMA (ecstasy) and methamphetamine (speed). In his clinic, he treats individuals with cocaine addiction, while in the lab he studies the psychological traits of addicted individuals and the effects the drug has on their brains.
Functional magnetic resonance imaging (fMRI) and diffusion tensor imaging (DTI) are two types of imaging methods Moeller uses to see into the addicted brain. FMRI is related to blood flow in the brain, as a measure of neural activity. Diffusion tensor imaging (DTI) is used, in both animal and clinical models, to visualize white matter, the fibrous connections between brain regions.
"The goals of this research are to gain a greater understanding of the alterations in brain structure and function that lead to addictions and whether these alterations could be targets for medication treatment," Moeller said.
Moeller and colleagues have determined that cocaine abuse damages white matter in the corpus callosum, the bridge of neurons joining the brain's two hemispheres. Moeller's goal is to find drugs that block or reverse this neurotoxic damage to the brain.
There are no FDA-approved medications for treating cocaine addiction, but Moeller's lab already has found success developing drug treatments for addiction.
In 2007, Moeller and his colleagues published a paper in the American Journal of Drug and Alcohol Abuse suggesting that the antidepressant Celexa (now available as a generic) may be effective in reducing cocaine use in cocaine-addicted individuals. In 2008, another paper from his colleagues showed that Levadopa, a dopamine precursor drug used to treat Parkinson's disease, may also be effective as a treatment for cocaine addiction when combined with behavioral therapies.
Impulsivity and addiction
Moeller also has used brain scanners, paired with questionnaires and computerized tests, to study the psychological traits of individuals with addictions. What he has found, from tests of impulse control, is that impulsivity has a major impact in cocaine addiction.
"This problem of impulsivity is broader than addiction," Moeller said. "Other disorders, including Parkinson's and traumatic brain injury, are also associated with problems of impulse control."
Parkinson's patients, for example, have been known to have trouble controlling their gambling and behavior in response to the drugs they take for their condition.
"Our focus is on impulsivity," Moeller said. "Before we got into impulsiveness as a factor in addictions, the focus was on craving. People thought if you could control the hunger for the drug, you could stop the addiction. Many times patients won't be craving the drug, but they are in the neighborhood where the drugs are, or someone offers and they see something that reminds them of the drug, and they can't resist the impulse."
Cocaine addiction is an impulse-control problem, Moeller suspects, not simply a craving. But does cocaine make people impulsive or does impulsivity put users at risk of becoming addicted? It's a chicken and an egg problem, Moeller said, in need of more investigation.
"As we develop more insight into the neurobiology of addictions we can develop more effective medications and behavioral programs to effectively treat addictions," he said.