Research sheds new light on impact of diabetes on the brain
Researchers from the University of Sheffield and Sheffield Teaching Hospitals NHS Foundation Trust have discovered diabetic nerve damage causes more harm in the brain than previously thought, shedding new light on the disease.
The new findings published in the Diabetes Care journal reveal the extent of damage patients suffering with the disease can endure in areas of the brain called 'grey matter' – a key component of the central nervous system which is involved in touch and pain sensory perception.
During the study, which involved patients with Type 1 and Type 2 diabetes, researchers used recent advances in ground breaking brain imaging and analyses methods to take detailed nerve assessments of the brain using magnetic resonance imaging (MRI) techniques.
This revealed that the volume of certain brain regions in people with diabetic neuropathy was significantly lower compared to those without the disease. Previous studies have shown that the impact of the disease on the brain is limited and isolated to outside areas of the brain considered to be peripheral to core functions in the body.
The breakthrough could pave the way for better assessment and monitoring of the disease, which affects around a third of people with diabetes. This, in turn, could lead to better treatments for sufferers in the future.
Diabetes patient Tracey Smythe, 45, of Parson Cross, Sheffield, admits she had little understanding of diabetic neuropathy – which affects up to a third of patients suffering with Type 1 and Type 2 diabetes – when she was first diagnosed with the illness five years ago.
Now she finds "living with the disease hard" and crippling pains from the illness stop her from doing the simplest things – including walking her two dogs, going to the supermarket alone and wearing clothes with zips and buttons.
"It affects all aspects of my life. I get shooting pains that take me off my feet. One time the pain lasted four and a half hours. I couldn't get up the stairs without using my arms to pull me up. I was in on my own, and I felt frightened and vulnerable. "
She added: "Even walking my two dogs is impossible as the pain increases when I'm walking. All the time I'm taking risk assessments on what I can and can't do. If I'm making a cup of tea I need to ask myself if I'm going to be alright.
"My hands get swollen and numb and I'm constantly getting pins and needles. My husband has to be there when I'm cooking, and I can't even bake a cake without him helping do the mix. Even the weather affects me, and if it gets too hot or cold I feel worse.
"Imagine you've gone out on a good night and worn the tightest pair of shoes, and the next day your feet are killing you. That's what it's like constantly living with diabetic nerve damage. I just wish there was more doctors could do to help people like me, which is why better understanding of the disease through research is vital."
The pioneering research, which will benefit patients like Tracey, was conducted by Dr Dinesh Selvarajah, a Senior Lecturer and Honorary Consultant in Diabetes at the Royal Hallamshire Hospital and a team from Sheffield Teaching Hospitals NHS Foundation Trust and University of Sheffield led by Professor Solomon Tesfaye and Professor Iain Wilkinson.
The research was funded by JDRF, the leading global funder of Type 1 diabetes research.
Dr Dinesh Selvarajah, of the Royal Hallamshire Hospital, said: "Diabetic nerve damage has a massive impact on the quality of people's lives, physically, mentally and socially.
"With the number of people suffering from diabetes around the world soaring, these are significant findings. Our study reveals for the first time how extensively involved diabetic neuropathy is in the brain, causing shrinking and a reduction in the main part of the brain associated with sensation. This is a new insight which will go a long way towards helping us better understand, treat and prevent a disease which we thought to be fairly innocuous in terms of effects on the brain.
"The next steps will be for us to investigate at what stage this occurs, what the consequences of this are and whether it can be prevented as it could be impacting on patient's behaviour and psychology."
Iain Wilkinson, an MR Physics Professor within Academic Radiology at the University of Sheffield and an Honorary Consultant Clinical Scientist for Sheffield Teaching Hospitals NHS Foundation Trust, said: "To see leading-edge MRI technology pinpoint changes that might play an influential factor in the quality of so many lives highlights the need for clinical research like this. It's such an important part of our Teaching Hospital and University.
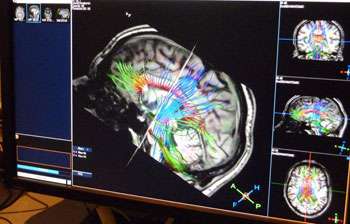
"MRI is such a useful neuroimaging tool in both medicine and patient-based medical research. The technique that we have been using is often termed 'volumetry' – recent scanner improvements enable the collection of high quality, high resolution, 3D datasets of the brain in an acceptable time, which, when coupled with the latest image processing systems, enable us to look at, or 'segment', different parts of the brain in patients who do or do not have diabetic neuropathy. The overall technique indicates where the differences that we are observing are occurring."
The grey matter region identified is a major component of the central nervous system, consisting of brain cells (or neurons) which process information from sensory organs in order to decide and execute functions. Loss of nerve cells in the grey matter, more properly known as cerebral atrophy, is highly undesirable as the functions of that area of the brain can become impaired.
















