New study identifies heart-specific protein that protects against arrhythmia
Researchers at the Cedars-Sinai Heart Institute have identified a heart-specific form of a protein, BIN1, responsible for sculpting tiny folds in pockets that are present on the surface of heart muscle cells. The study provides the first direct evidence of a previously theoretical "fuzzy space" or "slow diffusion zone" that protects against irregular heartbeats by maintaining an ideal concentration of electrochemical molecules.
"The findings help us understand how heart cells are organized, but more importantly, they give us insight into the way heart cells change when hearts start to fail," said Robin Shaw, MD, PhD, cardiologist and expert in heart failure and rhythm abnormalities at the Heart Institute.
"In addition, the results have diagnostic implications and eventually could lead to therapeutic options," said Shaw, senior author of an article in the May 18 issue of Nature Medicine that describes the study, which was conducted in laboratory mice. "By measuring the BIN1 level in the heart or in the bloodstream, we believe we can approximate the health of the heart and prognosticate patient outcome because we know BIN1 is decreased in heart failure. This gives us a target: If we can restore or replace the BIN1, perhaps we can rescue failing hearts."
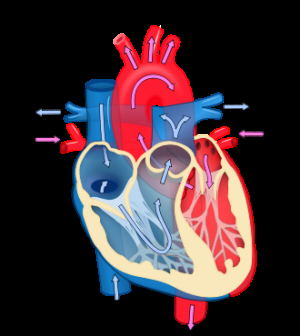
The surface of muscle cells in the main pumping chamber of the heart – the left ventricle – is dimpled like a golf ball, but the dimples form deep pockets called T-tubules. Molecules of electrically charged chemicals "linger" inside the tubules, waiting to rush through gated channels of the cell membrane into the cell. When calcium enters the cell, the heart cell contracts. An outflow of potassium molecules counteracts the calcium influx and allows the cell to relax.
Shaw's group, which has studied BIN1 for seven years, previously found that BIN1 allowed calcium channels to localize to the T-tubules, establishing pathways for calcium to get into the cell. They also found that BIN1 could be detected in the bloodstream as well as in the heart, that heart BIN1 is decreased by 50 percent in advanced stages of the most common forms of heart failure, and that low levels of BIN1 in the blood are a predictor of heart rhythm disturbances.
Heart researchers used to speculate that the BIN1 protein was responsible for making the T-tubules themselves, but Shaw's group found that the pockets exist even in the absence of the protein.
"In this study, using specialized microscopes, we could see that even though the T-tubules were still there, they looked very different. We discovered that although BIN1 does not create the tubule, it shapes it. The tubule was thought to be a very smooth dip of the membrane, but we now know there is a very complex folding, where BIN1 sculpts microfolds within the tubule," Shaw said.
"The tiny folds are very important because they can trap the chemicals that control heart rhythm," he added. "A little bit of trapping of calcium and potassium ions slightly changes the concentration of the environment just outside the cell, and these subtle changes are very protective for the heart. They actually alter the electrophysiology, protecting against arrhythmias like those that occur in heart failure. About 300,000 people die each year of heart failure, and rhythm abnormalities are the dominant cause of death."
The findings present a new perspective on heart failure development and rhythm abnormalities.
"We cardiologists historically have said, 'The heart gets big and loses its shape, and this somehow affects the electrical circuitry.' But this study suggests that even before the heart becomes enlarged, there is a decrease in BIN1. We knew loss of BIN1 predicted arrhythmia. Now we know why: Without BIN1, the protective microfolds go away," Shaw said. "We believe that when a patient's heart is stressed for any reason – heart attack, infection, disease – the 'program' within each heart cell changes – the genetic 'signaling' changes – and the cell gets the message to make less BIN1."
Shaw said cardiologists now use ultrasound images and estimates of the amount of blood pumped out of the left ventricle with each heartbeat to gauge the health of a patient's heart, but cardiologists long have known that this 'ejection fraction' is a poor indicator of patient well-being or outcome.
"The membranes of heart cells, like other cells, recycle, and thus heart cell membranes and their associated BIN1 gets into the bloodstream. By taking a simple blood sample, we can measure what's going on in the heart. As we refine this BIN1 blood test, we believe we will be able to do a biochemical assessment of the heart cell, the myocyte," Shaw said.
Shaw and his team identified the cardiac version of BIN1, but other variations affect other parts of the body. In the brain, for example, it is associated with Alzheimer's disease; in skeletal muscle, BIN1 loss is involved in muscular dystrophy. Slight differences in the BIN1 protein occur within genetic building blocks called exons, and the cardiac version has a signature that includes exons 13 and 17. The research team found that the binding of these two particular building blocks to the myocyte's internal structural proteins creates the cardiac membrane microfolds.
More information: Nature Medicine, "Cardiac Spliced BIN1 Folds T-tubule Membrane, Controlling Ion Flux and Limiting Arrhythmia," May 18, 2014. DOI: 10.1038/nm.3543