Demand for cheap food is to blame for widespread chicken contamination

More than two-thirds of chicken produced in the UK is contaminated with disease-causing bacteria, an investigation by The Guardian has revealed. Although the bug can be killed by proper cooking, it is estimated more than 300,000 people in the UK get diarrhoea from this bug every year. More than 100 people die as a consequence, and many more developing long term neurological and gastrointestinal problems.
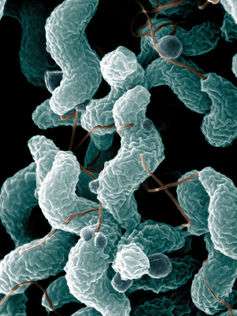
Despite the burden of disease caused by the bacteria called Campylobacter jejuni, it has remained "under the radar", unlike the scares caused by bacteria such as Salmonella and Listeria in the 1980s and 1990s. The problem of Campylobacter is on the top of the agenda for poultry producers and the Food Standards Agency (FSA) and a major concern for our major retailers, but The Guardian believes that not enough is being done.
The intensive nature of production, transport, slaughter and processing gives the bug many opportunities to spread through flocks and between carcasses. In a large chicken processing plant, 200,000 animals may be slaughtered and butchered each day.
If the first flock on the line that day has Campylobacter infection, then there is a good chance that many of the whole birds or chicken portions leaving the plant that day will be contaminated. Good hygiene, cleaning and following the correct procedures are vital in reducing these risks, but it would seem corners are being cut and errors are being made that impact directly on food safety.
How can the spread be controlled
Spread of Campylobacter is difficult to control in chicken production. Usually the bug survives in vast numbers in chickens' intestines. Although it can occasionally make chickens ill, it is normally carried with no observable effect on the bird.
The bug also spreads very quickly within a flock. It is not clear where Campylobacter comes from, though the practice of "thinning" is the single largest risk of a flock becoming infected. The practice involves selling lighter chicken for early slaughter to avoid overstocking, whilst retaining the remainder for slaughter at a greater weight.
The controls that have been successful in reducing Salmonella in chickens are less effective in reducing Campylobacter. There is also no vaccine available.
Some methods of controls are under investigation by FSA and the poultry industry. These include blast chilling, lactic acid treatment and bacteriophage treatment, but they are costly and in most cases of questionable efficacy.
Ultimately it is a difficult balance between providing cheap and nutritious food and maintaining food safety for an industry that operates on small margins. There is no specific legislation for Campylobacter control, such as there is for Salmonella control. Introducing any legislation will increase cost, which could push production overseas where chicken can be produced even more cheaply but where standards in hygiene and animal welfare are lower.
Longer-term solutions
Ultimately on-farm controls, such as vaccines or breeding of birds that are more resistant to Campylobacter infection, are likely to be more successful. However, these are some way off and need greater support from government and industry. The focus on quick solutions to meet FSA targets on reduction of carcass contamination has to an extent ignored long-term solutions.
Another worry is that emerging variants of Campylobacter are more likely to leave the gut and contaminate the liver or muscle. This would make controls after slaughtering even less effective as they would be unable to penetrate into the organs.
The question I am often asked is: "Do you eat chicken?" The answer is "yes … but I ensure that any chicken I eat is thoroughly cooked and I always practice good hygiene within the kitchen to avoid cross contamination". At present this is the best, and perhaps, the only thing that can be done to reduce the risk of Campylobacter infection.
This story is published courtesy of The Conversation (under Creative Commons-Attribution/No derivatives).![]()

















