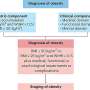
Impact of electronic personal health record on hypertension under study
Whether patients with an electronic handle on their health are more successful at beating one of the nation’s leading chronic diseases is under study.
The study, funded by the federal Agency for Healthcare Research and Quality, will give hundreds of patients with hypertension an electronic personal health record that enables them to post their blood pressure, weight, even what they eat in their medical record and e-mail their physicians when needed.
“From a chronic illness standpoint, the literature is pretty clear: The more involved and engaged I am in managing my own illness, the better my outcome,” says Patricia Sodomka, director of the Medical College of Georgia Center for Patient and Family Centered Care, senior vice president for patient and family centered care for MCG Health, Inc. and principal investigator on the $1.2 million grant. “It just makes common sense.”
MCG researchers will work with hypertensive patients in the family medicine and internal medicine practices at MCGHealth to see if the electronic personal health record enhances patient involvement.
“Our first measure is patient activation; if having ready access to information about yourself and to your physician makes you more activated as a patient and if you are more activated, does it lower your blood pressure,” says Dr. Peggy Wagner, research director for the MCG Department of Family Medicine and study co-investigator.
Two small studies will first get patient and physician input on how to make, IQHealth™, the electronic personal health record developed by Kansas City, Mo.-based Cerner Corp, more patient friendly.
A year-long study of 720 patients with hypertension will follow in which half the participants will use the newly-refined electronic personal health record and the remainder will receive standard treatment for a condition that affects about one quarter of the population or 65 million Americans.
“Hypertension, which is so pervasive in our society, is a great model because lifestyle has such an impact and the outcomes are relatively easy to measure,” Dr. Wagner says. “The hypothesis clearly is, if you have this electronic personal health record that is used by a patient and his primary care doctor, that the patient will be more likely to bring his hypertension under control.”
“Patient-care documentation systems today are dominantly in the hands of the providers and written from their perspective,” Mrs. Sodomka says. “The shift is toward shared information systems with patients and families, where patients and families can put their own information in there, their observations, their tracking, documenting things that are important to them. This is a shift that is being made in health care, a huge shift and this study is part of that. The idea is that if patients start really documenting things that are important them, if they start documenting what they are eating, for example, they will realize what they are eating and finally get control of their diet.”
The MCG Center for Patient and Family Centered Care, received a $30,000 grant from the Institute for Healthcare Improvement/Robert Wood Johnson Foundation in 2005 to test the Cerner system, used under the brand name My HealthLink at MCGHealth, in patients with multiple sclerosis. The 12-month study found that patients liked having a secure electronic link to care givers and that the electronic personal health record is an effective tool in helping battle chronic disease.
“An electronic personal health record is recognition that if we are serious about optimal outcomes in health care, we have to involve the patient,” says Dr. Charlotte Weaver, vice president and executive director for nursing research at Cerner. The company, a pioneer in the evolution of the electronic medical record and electronic personal health record, got patient input for the design of its system and looks forward to additional input to further refine the product, she says. Refinements likely will include feeding blood pressure measurements directly from the cuff to the electronic personal health record. Similar direct feeds with weight scales and even urine analysis via the toilet also are under development. “We are actively working on the integration of medical devices,” Dr. Weaver says.
“At the end of the day, if you can deliver a personal health record that people will use, that delivers just tremendous value to our health care system as well as to individuals,” Dr. Weaver says. Chronic diseases, such as hypertension, among aging baby boomers make the timing and impact significant, she says. “Cerner is pleased and honored to be a partner with the Medical College of Georgia in this important work.”
The Institute for Family Centered Care, headquartered in Bethesda, Md., also is a partner in gathering input on the Cerner system from patients and physicians in diverse geographic locations with experience using other personal health records
“This project will help demonstrate that when we partner with patients to really redesign the system of care, we will build the system in a way that works best for the people we serve,” says Beverley H. Johnson, the institute’s president and CEO. “I think the project creates a way to look over the next couple of years at how you get effective, sustained partnerships with families in place to make the care of higher quality which will lead to better outcomes.”
Study participants don’t have to have a computer; study coordinators will help those who don’t find where they can use one. However one of the many questions being asked is whether or not having a computer affects use of the electronic personal health record.
They will learn how to use the electronic record then have follow up visits at three, six and 12 months. Researchers will measure what they call patient activation or just how involved patients are in their own health, gather pertinent biological data such as blood pressure and waist circumference and use a widely accepted test to assess their relationship with their physician.
Source: Medical College of Georgia