Maternal obesity not strongly linked to obesity in offspring says study
Professor Debbie Lawlor and colleagues used two approaches to test the ‘developmental overnutrition’ hypothesis which asserts that if a woman is overweight during pregnancy, high sugar and fat levels in her body might permanently affect her growing baby’s appetite control and metabolism, thus increasing the child’s risk of becoming obese in later life.
First, the researchers asked whether offspring fat mass is more strongly related to maternal BMI than paternal BMI; it should be if the hypothesis is true.
Second, they asked whether a genetic indicator of maternal fatness – the “A” variant of the FTO gene – is related to offspring fat mass. A statistical association between maternal FTO genotype and offspring fat mass, after taking account of the offspring’s own FTO genotype, would support the developmental nutrition hypothesis.
The researchers used data from the Avon Longitudinal Study of Parents and Children (ALSPAC) to look for associations between the pre-pregnancy BMI of the parents of about 4,000 children and the children’s fat mass at ages nine to eleven years.
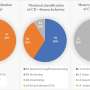
They found that both maternal and paternal BMI were positively associated with offspring fat mass but the effect of maternal BMI was greater than the effect of paternal BMI. However, the greater effect of maternal BMI was too weak to explain the recent obesity epidemic.
When the researchers examined maternal FTO genotypes and offspring fat mass, there was no statistical evidence to suggest that differences in offspring fat mass were related to the maternal FTO genotype.
Professor Lawlor said: “If true, the developmental over-nutrition hypothesis has wide-reaching public health implications as it means the obesity epidemic could accelerate across generations and continue to do so for some time, even with effective obesity prevention programmes.
“However, our study indicates that developmental overnutrition has not been a major driver of the recent obesity epidemic. Therefore, interventions that aim to improve people’s diet and to increase their physical activity levels could slow or even halt the epidemic.”
Source: University of Bristol