Cancer-causing protein can also help fight the tumors it causes
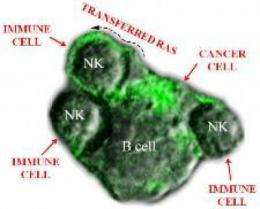
Oncogenes are genes that when mutated or expressed in high concentrations can cause normal cells to become cancerous. Now research from Tel Aviv University is demonstrating that Ras, one of the first oncogenes discovered, has the power to heal as well as harm.
Ph.D. student Oded Rechavi and his fellow researchers at Tel Aviv University's Department of Neurobiology have found that Ras has the ability to transfer from cancer cells into immune cells — such as t-cells — a transfer that may be the key to creating new drugs to fight cancerous tumors.
Prof. Yoel Kloog, dean of the university's Faculty of Life Sciences and a renowned expert in the field, is supervising the project. He and Rechavi published the discovery in the journal Public Library of Science One and a recent review about such cell-to-cell transferring of proteins in FEBS Letters.
Turning a cancer-causing protein against cancer itself
The idea that proteins can transfer between cells challenges the original theory of the cell, according to Rechavi. "All the energy flow, metabolism, and biochemistry of life is supposed to happen within the boundaries of an individual cell," he says. "Here we show that when cells in the immune system interact with other cells, proteins are exchanged without being secreted from the cell, and act in both the immune and original cells alike."
"When Ras transfers from one cell to another, it strengthens the immune system. The immune cell that adopts the mutated Ras gets activated and reacts against the cancerous cell that donated the Ras. This does not happen for advanced tumors, but if we could control the movement of Ras, we would have a better understanding of how immune cells react against cancer" and provide the scientific basis for an entirely new class of cancer drugs.
The researchers are working to discover the mechanisms by which the Ras protein is transferred, and initial results look promising. One current theory Rechavi is investigating is that the membranes of the cells temporarily fuse together. What is certain, however, is that once t-cells acquire mutated Ras, they are able to generate clones with the ability to respond against this specific threat.
"When immune cells scan their targets they bind to their targets," he says. "When immune cells acquire normal Ras, nothing happens. But when they acquire mutated Ras from a potential tumor, it starts a cascade. This results in the production of cytokines that help the immune system and act against the cancer."
Transferring potential into a drug
Rechavi says that understanding the nature of this interaction between mutated Ras and immune t-cells can unlock mysteries about the nature of proteins and cells. The next step is to identify other proteins that, like Ras, are able to transfer outside of their cell of origin.
Rechavi is now conducting a scan of proteins in an attempt to identify which ones have similar characteristics and abilities to Ras, and how they might transfer in the body. The TAU researchers have developed a technology to scan hundreds of proteins and have already discovered many with transferring properties; they plan to publish their results soon.
The more researchers learn, the more they can exploit these cells to keep the human body healthy — but Rechavi warns that not all the news may be good. "It could be that a bad protein is able to transfer from cancer cells to immune cells as well, upon acquiring such protein the immune system will be less active," says Rechavi. "It's also possible that a tumor could transfer the Ras protein into cells that normally support tumor growth, like stroma cells that grow blood vessels for the tumor. This is why we have to work to understand what is happening."
Source: Tel Aviv University (news : web)












