Scientists Find New Way to Get Physical in the Fight Against Cancer
(PhysOrg.com) -- Berkeley Lab researchers have shown that the biochemical activity of a key player in cancer metastasis can be altered by the application of a direct physical force. This new way in which cells can sense and respond to physical forces presents a new road for future cancer therapies.
Conventional biological wisdom holds that living cells interact with their environment through an elaborate network of chemical signals. As a result many therapies for the treatment of cancer and other diseases in which cell behavior goes awry focus on drugs that block or disrupt harmful chemical signals. Now, a new road for future therapies may have been opened with scientific evidence for a never seen before way in which cells can also sense and respond to physical forces.
A team of researchers with the Lawrence Berkeley National Laboratory (Berkeley Lab) and the University of California (UC) Berkeley has shown that the biochemical activity of a cellular protein system, which plays a key role in cancer metastasis, can be altered by the application of a direct physical force. This discovery sheds important new light on how the protein signaling complex known as EphA2/ephrin-A1 contributes to the initiation, growth and progression of cancerous cells, and also suggests how the activity of cancer cells can be affected by surrounding tissue.
“This first evidence that the EphA2/ephrin-A1 receptor-ligand complex, which was previously thought to be strictly a chemical sensor, can actually sense mechanical properties as well,” says chemist Jay Groves, who led this research. “This coupling of mechanical and chemical signaling, which could never have been seen with classical biological methods, helps explain some of the biological mysteries concerning the onset and progression of cancer.”
Groves holds a joint appointment with Berkeley Lab’s Physical Biosciences Division and UC Berkeley’s Chemistry Department. He is also a Howard Hughes Medical Institute (HHMI) investigator. With members of his research group Khalid Salaita and Pradeep Nair, plus Rebecca Petit, he has co-authored a paper on this research that was published in the March 12, 2010 issue of the journal Science. The paper is titled, “Restriction of Receptor Movement Alters Cellular Response: Physical Force Sensing by EphA2.” Other co-authors were Joe Gray, Richard Neve and Debopriya Das of Berkeley Lab’s Life Sciences Division.
Cancer and EphA2/ephrin-A1
The term “metastasis” comes from the Greek word for “displacement,” and it is used to describe the process whereby cancer cells detach from a tumor, enter the bloodstream and spread to other tissues throughout the body. For example, cancerous breast cells can spread to a lung and form a new breast cancer tumor there. Central to metastasis is the EphA2/ephrin-A1 receptor-ligand complex.
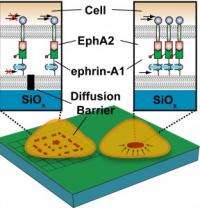
EphA2 is a member of the receptor tyrosine kinase (RTK) family of enzymes that are key regulators of cellular processes. The over-expression of EphA2 has been linked to a number of human cancers, including melanoma, lung, colon and prostate, but is especially prominent in breast cancer. Some 40-percent of all breast cancer patients show an over-abundance of EphA2, with the highest levels found in the most aggressive cancer cells. Ephrin-A1 is a signaling protein that is tethered to the surface of a cell’s outer membrane. It binds to EphA2 in a neighboring cell like a key fitted into a lock. When ephrin-A1 binds with EphA2, the newly bound complexes become activated and gather in a cluster.
“The host cell will then literally give the clusters a distinctive tug, applying a force that pulls the clusters across the surface of the cell to a centralized location,” Grove says. “What we found is that by applying an opposing force, we could alter the cell’s biochemical activity. When we applied a big opposing force we were able to convert highly invasive cells into well-behaved cells. This shows that in addition to chemically sensing the presence of ephrin-A1, the cells also sense the mechanical properties of the local environment in which ephrin-A1 is displayed.”
Spatial Mutation
Observations have indicated that mammalian cells are sensitive to the physical aspects of their environment, such as the texture or geometry of the surrounding tissue. However, evidence that physical forces impact freely-moving signaling molecules (as opposed to focal adhesion molecules) in the membranes of cells has been lacking because the cell membrane is an environment that has always been difficult to characterize and manipulate. Groves and his research group have found a way to overcome this obstacle with the development of unique synthetic membranes constructed out of lipids and assembled onto a substrate of solid silica that enables them to directly control cellular signaling activities.
“We call this approach the ‘spatial mutation’ strategy because molecules in a cell can be spatially re-arranged without altering the cell in any other way,” Groves says. “We first used this strategy in 2005 to study T cell signaling in the immune system.”
In this latest study, Groves and his colleagues worked with mammary epithelial cells from a library of 26 model human breast cancer cell lines that have been well-characterized by co-author Gray and his research groups at Berkeley Lab and UC San Francisco.
Says co-author Nair, “Gray’s research has demonstrated that this library substantially reproduces the genomic abnormalities and drug responsiveness of primary breast cancer tumor cells from patients, and constitutes the most comprehensive system for the study of the various aberrations responsible for human breast cancer.”
To test the sensitivity of the EphA2/ephrin-A1 signaling complex to mechanical forces, Groves and his group patterned their silica substrates with chromium metal lines that were 10 nanometers in height and 100 nanometers wide. These metal lines acted as diffusion barriers that impeded the lateral mobility of the EphA2/ephrin-A1 complexes in the synthetic membrane. The movement and spatial organization of the complexes were subsequently tracked through a combination of Total Internal Reflection Fluorescence (TIRF), reflection interference and epifluorescence imaging techniques.
“Without the barriers, the clusters of EphA2/ephrin-A1 signaling complexes were transported to the center of the cell-supported membrane junction, but with the barriers in place, there was an accumulation of clusters at the barrier boundaries,” Groves says. “This resulted in a spatial reorganization that altered the cell’s biochemical behavior.”
Quantitative analysis of these changes to the spatial organization of the EphA2/ephrin-A1 signaling complexes across the library of breast cancer cell lines revealed a strong correlation with the potential for metastasis. Since the patterned metal lines in the silica substrate are analogous to the stiffness, texture and other elastic and mechanical properties of tissue, as well as to internal structures within the cell membrane, the results of this study point to intriguing new possibilities for breast and other cancer therapies.
“It’s possible that the force-sensing process itself could provide a target for therapeutic intervention,” says Groves. “We’re also excited about finding targets for which there may be drugs that have already been developed but are now being used to treat diseases other than cancer. Given the sensitivity to mechanical forces displayed by the EphA2/ephrin-A1 signaling complexes, it is possible these existing drugs could be redirected to the treatment of cancer.”















