New study characterizes cognitive and anatomic differences in Alzheimer's disease gene carriers
In the most comprehensive study to date, neurologists have clearly identified significant differences in the ways that Alzheimer's disease (AD) affects patients with and without the apolipoprotein E ε4 gene (APOE ε4), a known genetic risk factor for the neurodegenerative disease, using a combination of cognitive and neuroanatomic measures. The study found that this gene influences the way the disease manifests, even at its mildest clinical stages.
Study highlights include:
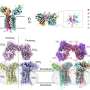
- Patients with mild AD who carry the ε4 form of the APOE gene perform more poorly on memory tests and have more prominent abnormalities in brain regions critical for memory, compared with patients without this gene variant.
- In contrast, patients with mild AD who do not have the APOE ε4 gene perform more poorly on tests of attention, language, and executive function and have more prominent abnormalities in brain regions critical for these abilities, compared to patients with APOE ε4.
Both APOE ε4 carriers and non-carriers displayed impaired memory in the study, but in qualitatively different ways. Researchers note that a variety of types of cognitive tests - tasks looking at memory, language, attention, and executive function - are necessary to make an early diagnosis and monitor of the progression of AD effectively. So far, the emphasis for early diagnosis and monitoring of AD has largely been on memory tests.
The study appears in the latest issue of the Proceedings of the National Academy of Sciences (PNAS).
Using data collected from the Alzheimer's Disease Neuroimaging Initiative, a large multi-center North American study of possible biomarkers for AD, neurologists from the Penn Memory Center at the University of Pennsylvania School of Medicine and the Massachusetts Alzheimer's Disease Research Center at Massachusetts General Hospital (MGH) and Harvard Medical School(HMS) examined how the presence or absence of the ε4 form of APOE influences cognitive function and brain anatomy measured from MRI scans.
Studying participants diagnosed with mild AD, the researchers compared the differences in cognition and in regional cortical atrophy of 67 APOE ε4 carriers with those of 24 non-carriers. Results from a biomarker test of cerebral spinal fluid, developed and previously reported by Penn Medicine researchers, was used to confirm with high diagnostic accuracy that patients included in the study had a molecular profile consistent with AD.
For future clinical trials, the researchers note that APOE genotype should be considered when analyzing the effects of possible treatments.
"A few recent clinical trials reported differences in the way patients responded to the drugs being tested depending on whether or not they carried the ε4 allele, which have prompted groups to study these populations independently," said senior author Bradford C. Dickerson, MD, associate professor of Neurology at MGH and HMS. "Rather than restricting trials exclusively to patients with or without APOE ε4, the results from this paper suggest that different behavioral and brain measures, dependent on participants' genotype, might be a useful approach to consider in evaluating investigational drugs."
Ultimately, a personalized medicine approach may factor an individual's genetic status in when considering how to diagnose and monitor the disease.