How the parasite responsible for severe forms of malaria can resist a major antimalarial agent
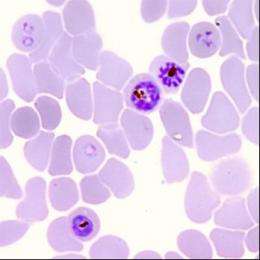
French esearchers from CNRS, INSERM and Toulouse University Hospital have demonstrated how the parasite Plasmodium falciparum, which causes severe forms of malaria, is able to circumvent the action of artemisinin and its derivatives, which are today the first-line drugs used to treat this disease.
This study supplies some important findings that will enable a clearer understanding of the mechanisms of resistance to antimalarial drugs and the testing of novel therapeutic strategies in a context where the drug resistance of parasites is of increasing concern. Published in the May 2010 issue of Antimicrobial Agents and Chemotherapy, this work was carried out in collaboration with the US National Institutes for Health (NIH).
Malaria still continues to kill nearly a million people each year throughout the world. There is no vaccine against this infectious disease caused by a parasite of the Plasmodium genus and propagated via the bites of certain mosquitoes. Plasmodium falciparum is the most pathogenic species, causing a high death rate. It accounts for more than 80% of cases of human malaria and is present in the tropical regions of Africa, Latin America and Asia.
For the past ten years, artemisinin (ART), a substance extracted from a Chinese plant, has become the first-line drug for malaria, particularly since other compounds have lost their efficacy. Its action against all strains of Plasmodium falciparum, including those resistant to other antimalarials, is the principal advantage of ART. Furthermore, its antimalarial activity is very rapid, and it has few adverse effects. Combining artemisinin with another antimalarial agents considerably reduces the risk of onset of resistance. For this reason, the WHO has for several years been recommending the systematic use of this compound and its derivatives in combination with other antimalarial agents. Artermisinin-based Combination Therapies (ACT) now constitute the most effective treatment for malaria, achieving a 95% cure rate.
However, in July 2009, the first cases of resistance to artesunate, the ART derivative most widely used in ACT, were observed among patients in South-East Asia. It has therefore become essential to determine how Plasmodium falciparum is able to circumvent the action of ART and its derivatives.
Thus the team led by Françoise Benoit-Vical, senior INSERM researcher in the CNRS Laboratoire de Chimie de Coordination, sought to isolate ART-resistant strains in an experimental manner. This feat was achieved at the end of 2009 when the scientists managed to obtain a strain of Plasmodium falciparum that was resistant to this compound and some of its derivatives, and the first to be adapted to in vitro culture. By furthering their investigations, the team was able to demonstrate that this ART-resistant strain was able to survive in the presence of ART at a dose that was 7000 times higher than the IC50 on susceptible strains. In addition, this experimental strain shared certain traits with the resistant strains found in the field.
The researchers also identified and characterized a new mode of parasite resistance. To evade the action of ART, Plasmodium falciparum arrested its development and entered a so-called state of quiescence. It thus functioned at a slow metabolic rate until the drug was eliminated. This quiescence phenomenon was only observed in parasites at the ring stage. In parallel, an analysis performed with a National Institutes of Health team suggested that the expression of some proteins involved in the cell cycle of Plasmodium falciparum might be modified in resistant strains. Further studies are planned to identify the genes responsible for the acquisition of ART resistance.
The scientists were thus able to demonstrate a novel resistance mechanism and now benefit from an important tool that will allow a clearer understanding of the mechanisms of resistance to antimalarial drugs; this will also enable the testing of different therapeutic options (new compounds, new therapeutic combinations, new targets, etc.).
More information: Increased tolerance to artemisinin in Plasmodium falciparum is mediated by a quiescence mechanism. Witkowski B, Leličvre J, López Barragán MJ, Laurent V, Su XZ, Berry A, Benoit-Vical F. Antimicrobial Agents and Chemotherapy. Mai 2010.














