Scientists find protein's bad guy role in prostate cancer
It's a disease affecting those closest to us – our fathers, brothers and sons.
Prostate cancer impacts one in six men in Canada. Last year, roughly 24,600 men were diagnosed with the disease.
Most types of prostate cancer are curable if caught and treated early. But little is understood about the mechanisms that cause a tumour to metastasize and spread to other parts of the body.
Damu Tang, an associate professor of medicine in the Division of Nephrology of the McMaster University's Michael G. DeGroote School of Medicine and St. Joseph's Healthcare Hamilton, has spent nearly a decade – and searched more than a million genes – to better understand the molecular underpinnings of prostate cancer progression.
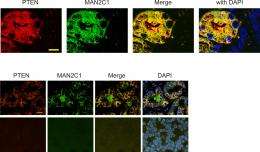
His research, published today in Nature Communications, shows for the first time the role of a specific protein – MAN2C1 – in prostate cancer development. The finding is significant because prostate cancer patients with increased levels of MAN2C1 appear to face more aggressive forms of the disease.
"This research could serve a diagnostic purpose in terms of likelihood of whether prostate cancers at early stages will progress into metastatic tumours," said Tang, who has a joint appointment in the Division of Urology, Department of Surgery at McMaster. "Patients with high levels of MAN2C1 may need more aggressive therapies when their cancers are still at early stages in order to prevent the development of metastatic cancer."
It's been known for some time that another protein, PTEN, is a powerful tumour suppressor. Clinical observations have shown that half of advanced prostate cancers either have no PTEN or reduced PTEN function.
Tang and his research team set out to understand how PTEN function becomes impaired in advanced prostate cancers. In the process, they discovered MAN2C1 and the role it plays in reducing PTEN function.
The research group found increases in the MAN2C1 protein in PTEN-positive prostate cancer cells dramatically increased the likelihood of cancers forming in mice. Additional research showed that in 659 prostate cancer patients, approximately 60 per cent of their prostate tumors had normal PTEN. Among these tumors, 80 per cent had increased MAN2C1.
The researchers concluded that increases in MAN2C1 in PTEN-positive prostate cancers enhance prostate cancer recurrence, meaning that patients with high levels of MAN2C1 have an increased risk of their tumors developing into metastatic cancer.
The next step for the researchers will be to look for ways to block the ability of MAN2C1 to impair PTEN function, Tang said. That could lead to the development of new therapies for patients with prostate cancer.













