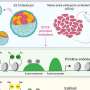
Noninvasive method accurately and efficiently detects risk of Down syndrome
Using a noninvasive test on maternal blood that deploys a novel biochemical assay and a new algorithm for analysis, scientists can detect, with a high degree of accuracy, the risk that a fetus has the chromosomal abnormalities that cause Down syndrome and a genetic disorder known as Edwards syndrome. The new approach is more scalable than other recently developed genetic screening tests and has the potential to reduce unnecessary amniocentesis or CVS. Two studies evaluating this approach are available online in advance of publication in the April issue of the American Journal of Obstetrics & Gynecology (AJOG).
Diagnosis of fetal chromosomal abnormalities, or aneuploidies, relies on invasive testing by chorionic villous sampling or amniocentesis in pregnancies identified as high-risk. Although accurate, the tests are expensive and carry a risk of miscarriage. A technique known as massively parallel shotgun sequencing (MPSS) that analyzes cell-free DNA (cfDNA) from the mother's plasma for fetal conditions has been used to detect trisomy 21 (T21) pregnancies, those with an extra copy of chromosome 21 that leads to Down syndrome, and trisomy 18 (T18), the chromosomal defect underlying Edwards syndrome. MPSS accurately identifies the conditions by analyzing the entire genome, but it requires a large amount of DNA sequencing, limiting its clinical usefulness.
Scientists at Aria Diagnostics in San Jose, CA developed a novel assay, Digital Analysis of Selected Regions (DANSR™), which sequences loci from only the chromosomes under investigation. The assay requires 10 times less DNA sequencing than MPSS approaches.
In the current study, the researchers report on a novel statistical algorithm, the Fetal-fraction Optimized Risk of Trisomy Evaluation (FORTE™), which considers age-related risks and the percentage of fetal DNA in the sample to provide an individualized risk score for trisomy. Explains author Ken Song, MD, "The higher the fraction of fetal cfDNA, the greater the difference in the number of cfDNA fragments originating from trisomic versus disomic [normal] chromosomes and hence the easier it is to detect trisomy. The FORTE algorithm explicitly accounts for fetal fraction in calculating trisomy risk."
To test the performance of the DANSR/FORTE assay, Dr. Song and his colleagues evaluated a set of subjects consisting of 123 normal, 36 T21, and 8 T18 pregnancies. All samples were assigned FORTE odd scores for chromosome 18 and chromosome 21. The combination of DANSR and FORTE correctly identified all 36 cases of T21 and 8 cases of T18 as having a greater than 99% risk for each trisomy in a blinded analysis. There was at least a 1,000 fold magnitude separation in the risk score between trisomic and disomic samples.
In a related study, researchers from the Harris Birthright Research Centre for Fetal Medicine, Kings College Hospital, University of London and the University College London Hospital, University College London, provided 400 maternal plasma samples to Aria for analysis using the DANSR assay with the FORTE algorithm. The subjects were all at risk for aneuploidies, and they had been tested by chorionic villous sampling. The analysis distinguished all cases of T21 and 98% of T18 cases from euploid pregnancies. In all cases of T21, the estimated risk for this aneuploidy was greater than or equal to 99%, whereas in all normal pregnancies and those with T18, the risk score for T21 was less than or equal to 0.01%.
"Combining the DANSR assay with the FORTE algorithm provides a robust and accurate assessment of fetal trisomy risk," says Dr. Song. "Because DANSR allows analysis of specific genomic regions, it could be potentially used to evaluate genetic conditions other than trisomy. The incorporation of additional risk information, such as from ultrasonography, into the FORTE algorithm warrants investigation."
Kypros H. Nicolaides, MD, senior author of the University of London study, suggests that fetal trisomy evaluation with cfDNA testing will inevitably be introduced into clinical practice. "It would be useful as a secondary test contingent upon the results of a more universally applicable primary method of screening. The extent to which it could be applied as a universal screening tool depends on whether the cost becomes comparable to that of current methods of sonographic and biochemical testing."
Dr. Nicolaides also notes that the plasma samples were obtained from high-risk pregnancies where there is some evidence of impaired placental function. It would also be necessary to demonstrate that the observed accuracy with cfDNA testing obtained from the investigation of pregnancies at high-risk for aneuploidies is applicable to the general population where the prevalence of fetal trisomy 21 is much lower. "This may well prove to be the case because the ability to detect aneuploidy with cfDNA is dependent upon assay precision and fetal DNA percentage in the sample rather than the prevalence of the disease in the study population," he concludes.
More information: “Non-Invasive Prenatal Detection and Selective Analysis of Cell-free DNA Obtained from Maternal Blood: Evaluation for Trisomy 21 and Trisomy 18,” by A.B. Sparks, C.A. Struble, E.T. Wang, K. Song, and A. Oliphant (DOI: 10.1016/j.ajog.2012.01.030). It will appear in the American Journal of Obstetrics & Gynecology, Volume 206, Issue 4 (April 2012).
“Chromosome-Selective Sequencing of Maternal Plasma Cell-Free DNA for First-Trimester Detection of Trisomy 21 and Trisomy 18,” by G. Ashoor, A. Syngelaki, M. Wagner, C. Birdir, and K.H. Nicolaides (DOI: 10.1016/j.ajog.2012.01.029). It will appear in the American Journal of Obstetrics & Gynecology, Volume 206, Issue 4 (April 2012).