Why resist insulin? Finding genes associated with insulin resistance
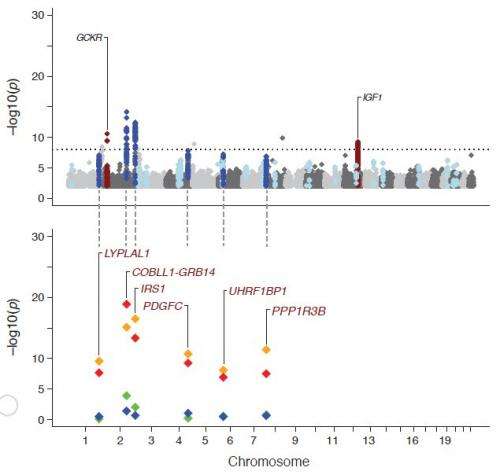
(Medical Xpress) -- Researchers have uncovered six genetic regions that appear to affect resistance to the effects of insulin, which is important in many cases of type 2 diabetes. Previously, only two regions had been described.
The team were able to identify the regions because they made allowance for obesity of the study participants: differences in obesity might otherwise have masked the effect of genetic variants that influence insulin resistance.
Worldwide, more than 350 million people have type 2 diabetes, and this number is increasing rapidly. People with diabetes either secret insufficient amounts of insulin, a hormone that controls blood sugar levels, or are resistant to its actions.
Previous studies have identified many genes associated with type 2 diabetes and insulin secretion, but little is known about the genetic basis of insulin resistance. This is surprising, because the heritability of insulin resistance has clearly been demonstrated in family and twin studies.
"Insulin resistance, diabetes and obesity are intricately linked in networks of interactions," says Dr. Inês Barroso from the Wellcome Trust Sanger Institute. "We know that insulin resistance has a significant genetic component and we hypothesized that the degree of adiposity might mask or modify the association between genetic variants and insulin resistance traits. We wanted to see if we might uncover novel variants if we accounted for the effects of body mass index.
"Our approach succeeded: We found six novel regions associated with insulin resistance. These regions should help us to characterize further the causes of type 2 diabetes."
We know that obesity is a major risk factor for insulin resistance. It is possible that the strong influence of obesity 'masks' the comparatively smaller genetic effects on insulin resistance that remain to be discovered. In addition, the risk of developing insulin resistance in a person who is genetically susceptible may differ depending on whether or not they are obese.
The research was carried out by a consortium of scientists affiliated with more than 150 institutions, who examined almost 100,000 samples. Researchers in the consortium (MAGIC: the Meta-Analyses of Glucose and Insulin-related traits Consortium) work collaboratively to identify novel genetic regions that influence glucose and insulin levels and other metabolic traits. It is the scale of this study that allowed the team to look at genetic effects on glucose and insulin levels across the whole genome: they accounted for differences in obesity levels between study participants while at the same time testing whether these genetic effects were different in people of different body size.
"Applying this method on a large scale we identified six genetic variants not previously known to be associated with insulin levels," explains Dr Claudia Langenberg, lead author on the study from the MRC Epidemiology Unit in Cambridge. "We also found that individuals carrying these risk variants had higher triglyceride and lower high-density lipoprotein cholesterol levels, linking these different features of insulin resistance.
"Our findings highlight the importance of taking body weight into consideration when studying the genetic basis of insulin resistance and its role for type 2 diabetes. The application of our statistical method can be useful for future genome-wide studies of other diseases that are strongly influenced or vary by known risk factors, such obesity, smoking or others."















