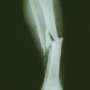
Spondylolisthesis linked to spinous process fractures
(HealthDay) -- There is a strong association between degenerative spondylolisthesis and spinous process fracture in patients undergoing interspinous process spacer (IPS) surgery, according to a study published online May 24 in The Spine Journal.
To investigate the risk factors associated with early spinous process fracture after IPS surgery, David H. Kim, M.D., from the Tufts University School of Medicine in Boston, and colleagues prospectively studied 39 consecutive patients with lumbar stenosis and neurogenic claudication undergoing IPS surgery. Participants underwent dual-energy X-ray absorptiometry scans, lumbar spine computed tomography (CT), and plain radiographs before surgery. Repeat CT imaging was performed within six months of surgery, and serial radiographs were performed at two weeks, six weeks, three months, six months, and one year post-surgery.
The researchers found that IPS surgery was performed on 38 patients at 50 levels (38 at L4 to L5, 12 at L3 to L4; 26 one-level, 12 two-level). CT identified 11 spinous process fractures in 11 patients, with no fractures seen on plain radiographs. Among patients with fractures, spondylolisthesis was observed on 100 percent of the preoperative radiographs, compared with 33.3 percent (nine of 27) of patients without fracture (P = 0.0001). Overall, 21 of 39 patients had spondylolisthesis, and the fracture rate among this group was 52 percent. None of the patients without spondylolisthesis had fractures.
"Degenerative spondylolisthesis appears strongly associated with the occurrence of spinous process fracture after IPS surgery," the authors write.
Several authors disclosed financial ties to medical device companies, including Lanx and Medtronic, whose implants were utilized in this study.
More information:
Abstract
Full Text (subscription or payment may be required)
Copyright © 2012 HealthDay. All rights reserved.