Scientists first to see trafficking of immune cells in beating heart
Blood flow to the heart often is interrupted during a heart attack or cardiac surgery. But when blood flow resumes, the heart may still falter. That's because collateral damage can occur as blood re-enters the heart, potentially slowing recovery and causing future cardiac troubles.
Researchers investigating this type of secondary heart damage have been stymied by the inability to see in real time how restoring blood flow leads to inflammation that can cause further injury. Now, working in mice, surgeons and scientists at Washington University School of Medicine in St. Louis, have captured the first images of a beating heart at a resolution so detailed they can track individual immune cells swarming into the heart muscle, causing inflammation.
The achievement is detailed in the July issue of the Journal of Clinical Investigation.
The researchers say that the imaging technique, called intravital two-photon imaging, is a powerful tool for understanding the inflammation that occurs when blood flow to the heart is temporarily stopped and later restarted.
"Inflammation is quite common after a heart attack, open-heart surgery, heart transplants and in atherosclerosis, and it can severely hamper recovery and lead to death," says senior author Daniel Kreisel, MD, PhD, a Washington University cardiothoracic surgeon who operates at Barnes-Jewish Hospital. "But little is known about how inflammation ramps up in the heart. Now that we have the ability to see all the cellular players involved, we can begin to think about new therapeutic targets for treatment."
Two-photon imaging has been used to image other organs in living mice but never the heart. Scientists had assumed that the flutter of the beating heart, which pulses about 500 times a minute in a mouse, would blur any images of individual cells.
"No one thought we could get clear images of cells inside the beating heart," says Wenjun Li, MD, research instructor of surgery and co-lead author with Ruben Nava, MD, and Alejandro Bribriesco, MD, both surgical residents at Barnes-Jewish Hospital. "But the images we captured are incredibly rich in detail, right down to the level of single cells. We think the principles underlying inflammation in the mouse heart will be applicable to humans."
One advantage of two-photon microscopy is the ability to penetrate deep into tissue, allowing scientists to image cells in the heart tissue.
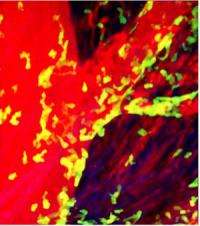
Using the technique in mice that had undergone heart transplants or had a blood flow to the heart temporarily interrupted, the researchers saw that within minutes of restoring blood flow, specialized white blood cells, called neutrophils, rushed into the heart. (To see a video of neutrophils, shown in green, swarming into the beating heart of a mouse after a heart transplant, click here.)
Neutrophils are known to be a key driver of inflammation but scientists had never seen the trafficking of immune cells as they move from the circulation into the heart muscle, where the cells formed large clusters that cause tissue damage.
In addition, by blocking neutrophils from blood vessel walls, the researchers could markedly reduce the movement of these cells into the heart, preventing further injury.
Kreisel, Li and their colleagues collaborated with co-senior author Mark Miller, PhD, an assistant professor of pathology and immunology, who pioneered the use of two-photon microscopy for studying the trafficking of white blood cells in living mice. Together, they developed a way to stabilize the beating heart so they could obtain high-quality images of immune cell trafficking.
The same team also has used the technique to image immune cells in mouse lungs, which also move as the mice breathe but not to the same extent as the heart. And other scientists have used two-photon imaging to watch neutrophils travel into the skin, liver and other organs. Surprisingly, the researchers are finding that the trafficking of neutrophils differs from one organ to the next.
"Each organ seems to have its own requirements for signaling and attracting inflammatory cells," says Kreisel, who also is an associate professor of surgery. "It is as if each organ has its own zip code. Now, we have the ability to identify all the cells and signaling molecules that play a part in heart inflammation and can block particular pathways to see if we can prevent organ damage."