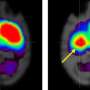
Melatonin pre-treatment is a factor that impacts stem cell survival after transplantation
When melatonin, a hormone secreted by the pineal gland, was used as a pre-treatment for mesenchymal stem cells (MSCs) prior to their transplantation into the brains of laboratory animals to repair damage from stroke, researchers in China found that the stem cells survived longer after transplantation. Previous studies had shown that 80 percent of transplanted MSCs died within 72 hours of transplantation. By contrast, the melatonin pre-treatment "greatly increased" cell survival, said the researchers.
The study appears as an early e-publication for the journal Cell Transplantation.
The pineal gland is a small endocrine gland located in the center of the brain, but outside of the blood–brain barrier. The melatonin it secretes acts as a signal and forms part of the system that regulates the sleep–wake cycle by chemically causing drowsiness and lowering body temperature. Melatonin is also known to be a powerful antioxidant and has been used clinically to treat sleep disorders.
In this study, the researchers used a melatonin pre-treatment on MSCs they harvested from the laboratory animals that had been chemically modeled with ischemic brain injury (stroke). Previous studies had shown that MSCs "express" melatonin receptors M1 and M2.
"Mesenchymal cells can be harvested from self-donors (autologous) without ethical concerns," said study co-author Dr. Guo-Yuan Yang of the Neuroscience and Neuroengineering Research Center at the Shanghai Jiao Tong University in Shanghai, China. "Studies have shown that MSCs differentiate into various cells and can, upon transplantation, improve functional recovery after ischemic brain injury. In this study we used laboratory rats chemically modeled with stroke and tried to determine if pretreatment with melatonin would promote cell survival."
Researchers transplanted pre-treated MSCs into one group of brain injured rats and also used a control group of animals that received MSCs that were not pre-treated with melatonin.
Study results demonstrated that the melatonin pre-treated MSCs had "enhanced survival under oxidative stimulation by activating the Erk1/2 pathway" (extracellular signal-regulated kinases), a chain of proteins in the cell that communicates a signal from a receptor on the surface of the cell to the DNA in the nucleus of the cell.
"Our study demonstrated increased survival of transplanted MSCs and revealed that the pre-treated MSCs reduced infarct volume and improved neurobehavioral outcomes for at least 14 days," said Dr. Yang.
The researchers noted that the impact of pre-treatment with melatonin was not MSC differentiation, and that development into mature brain cells was not an important factor in the beneficial effects derived from transplantation of either the untreated or the pre-treated cells. They suggested that the transplantation of MSCs pre-treated with melatonin may have a positive impact on the secretion of vascular endothelial growth factor (VEGF). VEGF is a signal protein produced by cells that stimulate vascular and blood vessel growth that can help restore the oxygen supply to tissues when blood circulation is inadequate.
"Our study demonstrated that melatonin pre-treatment promoted MSC survival in the laboratory setting and augmented the therapeutic efficiency of MSCs in the rat brain. The protective effect of melatonin is achieved by activation of the Erk1/2 pathway," they concluded. "This strategy of pre-treating stem cells may represent a safe approach for improving the beneficial effects of stem cell therapy for cerebral ischemia."
"It is important to identify factors that can impact on the survival of stem cells following their potential therapeutic use for a variety of neurological disorders", said Dr. Shinn-Zong Lin, professor of Neurosurgery and superintendent at the China Medical University Hospital, Beigang, Taiwan. "This study suggests that melatonin pretreatment could be a factor and its role should be explored further with other disease models and other cell types".
More information: www.ingentaconnect.com/content … re-prints/ct0998tang