December 24, 2013 report
Researchers identify risks for death from H7N9 avian flu virus
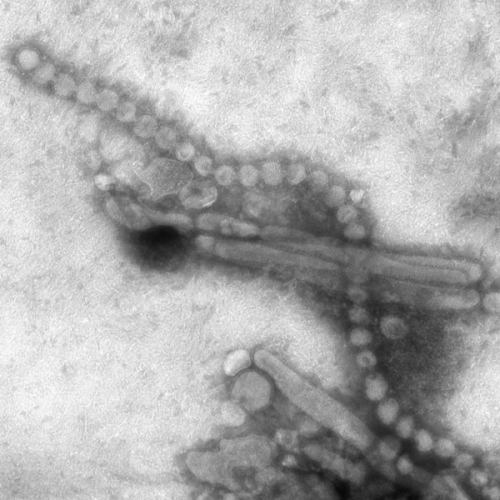
(Medical Xpress)—Since March 2013, the avian flu virus H7N9 has infected 134 people and caused 44 deaths. Among those infected, many, but not all, patients develop severe symptoms, including pneumonia and acute respiratory distress syndrome (ARDS), that can eventually result in death. Until now, scientists have not understood why the disease affects some more severely than others. Peter Doherty and his colleagues have found that patients with high levels of certain cytokines are more likely to suffer severe lung and airway damage than patients with lower levels of these cytokines. They also discovered that patients who carry a particular variant of the gene that codes for the protein IFITM3 are more likely to suffer severe symptoms and to die than patients with other versions of the gene. The research appears in the Proceedings of the National Academy of Sciences.
Previous research has shown that H7N9 patients with elevated plasma cytokine levels tend to experience poor outcomes. To study the relationship between cytokine levels and disease progression further, Doherty and his team took blood plasma samples from 18 patients infected with H7N9 who were admitted to the Shanghai Public Health Clinical Center. Eventually, 12 of the patients recovered and six died. The researchers found that blood levels of the cytokines Il-6 and Il-8 were 10 times higher than normal in all of the patients who died. Only one of the patients who survived had such high levels of these cytokines. The patients who died also had elevated levels of the cytokines IL-10 and macrophage inflammatory MIP -1β.
The team also examined samples from bronchoalveolar lavages performed on three of the patients, all of whom died. Concentrations of the cytokines IL-1β, IL-6, and IL-8 were one thousand times higher than normal, while concentrations of MIP-1α and MIP-1β were one hundred times higher than normal.
When the team sequenced the subjects' DNA, they found that patients with a variant of the gene that codes for IFN-induced transmembrane protein-3 (IFITM3), known as IFITM3 C/C, suffered more severe symptoms, required medical intervention sooner and were less likely to survive than patients with the variants IFITM3 T/C and IFITM 3 T/T. IFITM3 can prevent flu virus particles from entering the cytoplasm and thus prevent the virus from replicating. Subjects with the C/C variant had higher plasma levels of IL-6, IL-8, and MIP-1β. During the 2009 H1N1 avian flu outbreak, patients with the C/C variant also had elevated plasma cytokine levels and experienced worse outcomes.
The researchers suggest that screening for the IFTM3 genotype and monitoring of plasma cytokine levels can help ensure that patients diagnosed with H7N9 infection receive proper treatment.
More information: Early hypercytokinemia is associated with interferon-induced transmembrane protein-3 dysfunction and predictive of fatal H7N9 infection, PNAS, Published online before print December 23, 2013, DOI: 10.1073/pnas.1321748111
Abstract
A unique avian-origin A/H7N9 influenza virus has so far caused 134 cases with 44 deaths. Probing the host factors contributing to disease severity, we found that lower levels of plasma inflammatory cytokines on hospital admission correlated with faster recovery in 18 patients with A/H7N9 influenza virus, whereas high concentrations of (in particular) IL-6, IL-8, and macrophage inflammatory protein-1β were predictive of a less favorable or fatal outcome. Analysis of bronchoalveolar lavage samples showed up to 1,000-fold greater cytokine/chemokine levels relative to plasma. Furthermore, patients with the rs12252-C/C IFN-induced transmembrane protein-3 (IFITM3) genotype had more rapid disease progression and were less likely to survive. Compared with patients with the rs12252-T/T or rs12252-T/C genotype of IFITM3, patients with the C/C genotype had a shorter time from disease onset to the time point when they sought medical aid (hospital admission or antiviral therapy) and a shorter interval to development of the acute respiratory distress syndrome stage (reflected by shorter intervals between clinical onset and methylprednisolone treatments and higher rates of mechanical ventilator use), as well as experiencing elevated/prolonged lung virus titers and cytokine production and higher mortality. The present analysis provides reported data on the H7N9 influenza-induced "cytokine storm" at the site of infection in humans and identifies the rs12252-C genotype that compromises IFITM3 function as a primary genetic correlate of severe H7N9 pneumonia. Together with rs12252 sequencing, early monitoring of plasma cytokines is thus of prognostic value for the treatment and management of severe influenza pneumonia.
© 2013 Medical Xpress