Decline of antibiotic use among kids seems to be leveling off
(HealthDay)—A downward trend in antibiotic use among children may have leveled off in certain areas of the United States, a new study shows.
Researchers from Boston Children's Hospital and Harvard Medical School reviewed data from three health plans across the country—in New England, the Midwest and the Mountain West—from 2000 to 2010 to better understand how antibiotics are being prescribed in children and to learn if use is still dropping.
"This latest report finds that the decline in antibiotic use may have leveled out," said Dr. Louise Elaine Vaz, a clinical fellow in pediatric infectious disease and a health services research fellow at Boston Children's Hospital.
The 10-year study included children between the ages of 3 months and 18 years. The researchers collected information on diagnoses as well as the type of antibiotics used, although certain antibiotics and some topical forms were excluded.
The overall annual antibiotic-dispensing rates in each age group and each health plan were lower from 2009 to 2010 than they were from 2000 to 2001, but there wasn't a straight downward trend, Vaz said.
In the early part of the decade, rates declined relatively rapidly, particularly in the youngest age group—children younger than 3 years. Later in the decade, this decline slowed and even reversed in the 12- to 18-year-old age group, Vaz said. Children aged 3 and under were the highest users of antibiotics in all years of the study.
Antibiotic dispensing varied a lot between the three health plans, said Vaz, but the Mountain West group consistently had lower visit rates and antibiotic-dispensing rates compared to the other two.
The findings were published in the February issue of the journal Pediatrics.
"When we saw that the rates were leveling off, our next question was: Are there ways that we can still improve?" Vaz said.
"I think one of the interesting things we saw was that one health plan was a low prescriber," she said. "That ... suggested that although the rates are stabilized, some plans have lower prescribing rates than others and we may not have reached our optimal prescribing level."
One expert agreed.
"The study shows we've chipped away at the problem," said Dr. Wendy Sue Swanson, executive director of digital health at Seattle Children's Hospital. "In clinic, I don't feel the pressure from parents any longer the way I did in medical school when they were coming in looking for an antibiotic cure. I believe the public is more informed, but I think this data serves as a moment of pause."
In a commentary accompanying the study, Dr. Ateev Mehrotra, from the department of health care policy at Harvard Medical School, said some of the decline in use is due to better education about antibiotic overuse and to vaccines for pneumonia and the flu. But he said experts shouldn't get too comfortable with the news.
"While efforts to reduce over-prescribing of antibiotics have been successful over the last 20 years—roughly a 25 percent drop in antibiotics prescribed per child—the new study offers a cautionary note," he said.
Prescriptions are leveling off, but there is still overuse of broad-spectrum antibiotics, Mehrotra said.
Limiting over-the-phone prescriptions, cutting back on prescriptions for viral infections that do not clear up with antibiotics and encouraging parents to do more to treat their kids at home would help continue the downward trend in overuse, Mehrotra said in his commentary.
Swanson said she likes the idea of parents treating at home, but that doesn't mean parents have to feel alone. They can run questions by their doctor in a new way, she said.
"I'm such a technology enthusiast. Maybe we can get a mom on for a Skype visit or on email," Swanson said. "I think it's the beginning of something that allows patients and families to be stewards of their own health."
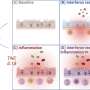
Swanson also said more doctors should consider pain relievers as the first line of defense against ear infections. In the study, ear infections were the most common reason for prescribing an antibiotic, accounting for more than 60 percent of all antibiotic prescriptions for kids under age 6.
There are many avenues for future research, Vaz said.
"We can learn why these differences persist in terms of geographic variation, and really hone in on how we can improve prescribing behavior," Vaz said. "I would love to see what's going on in these low-prescribing areas."
More information: Visit Seattle Children's Hospital for more on antibiotic over-prescribing.
Abstract
Full Text (subscription or payment may be required)
Copyright © 2014 HealthDay. All rights reserved.