February 13, 2014 report
Rare form of leukemia found to originate in stem cells
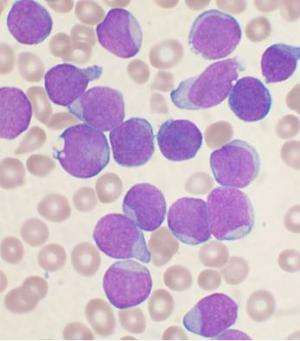
(Medical Xpress)—An international team of researchers working out of the University of Toronto has found that one type of rare leukemia appears to get its start in stem cells. In their paper published in the journal Nature, the team describes how they were able to identify haematopoietic stem cells and what it may mean for future treatment of the cancer. Nicole Potter and Mel Greaves offer an in-depth explanation of the work done by the team in a News & Views piece in the same journal.
Leukemia is cancer of the bone marrow or blood—it presents itself as an overabundance of white blood cells that have not matured. Because they are not able to carry out normal blood functions, the patient, if left untreated, dies because the properly functioning cells are crowded out by the cancerous cells. One rare type of leukemia, called acute myeloid leukemia (AML) is unique in that it gets its start in the blood forming tissues within bone marrow—it's also particularly aggressive.
Scientists have known about stem cells that eventually form into white or red blood cells (or platelets) for a couple of decades, what's new in this study is the identification of a specific type of stem (haematopoietic) cell that appears to at times mutate, causing AML, and that it tends to appear as a result of mutations of a specific gene—DNMT3a.
Research by the team has revealed that up to 25 percent of AML patients have the mutation—they've found that in addition to causing cancerous cells to develop, it also causes the (pre-leukemic) stem cells to behave in ways similar to cells that develop into normal blood cells, which allows for surviving chemotherapy. That means that a patient diagnosed with leukemia, who goes through chemo which results in remission of the leukemia, could find themselves having a relapse—that it happens, is obviously very bad news for patients, but that the researchers have uncovered how the pre-leukemic cells come to exist and how they survive is very good news. It means that tests can be developed to look for the mutated gene and then therapies developed that can target the specific hematopoietic stem cells before they mature into cancerous cells.
More information: Identification of pre-leukaemic haematopoietic stem cells in acute leukaemia, Nature (2014) doi:10.1038/nature13038
Abstract
In acute myeloid leukaemia (AML), the cell of origin, nature and biological consequences of initiating lesions, and order of subsequent mutations remain poorly understood, as AML is typically diagnosed without observation of a pre-leukaemic phase. Here, highly purified haematopoietic stem cells (HSCs), progenitor and mature cell fractions from the blood of AML patients were found to contain recurrent DNMT3A mutations (DNMT3Amut) at high allele frequency, but without coincident NPM1 mutations (NPM1c) present in AML blasts. DNMT3Amut-bearing HSCs showed a multilineage repopulation advantage over non-mutated HSCs in xenografts, establishing their identity as pre-leukaemic HSCs. Pre-leukaemic HSCs were found in remission samples, indicating that they survive chemotherapy. Therefore DNMT3Amut arises early in AML evolution, probably in HSCs, leading to a clonally expanded pool of pre-leukaemic HSCs from which AML evolves. Our findings provide a paradigm for the detection and treatment of pre-leukaemic clones before the acquisition of additional genetic lesions engenders greater therapeutic resistance.
© 2014 Medical Xpress