March 20, 2014 report
Study shows amount of vitamin A during pregnancy affects offspring immunity
(Medical Xpress)—A team of researchers working in the Netherlands has found that the amount of vitamin A a woman consumes during pregnancy has a lifelong impact on the immune system of her offspring. In their paper published in the journal Nature, the team describes experiments they conducted with pregnant mice on vitamin A restricted diets and the impact it had on the development of offspring immunity. In a companion News & Views article Gérard Eberl, of the Pasteur Institute provides a history of vitamin A research and the various findings of several research efforts.
Medical scientists have known for some time that vitamin A is important both for a developing fetus and for people of all ages, a lack of it has been linked to blindness, reproduction problems, bone metabolism and skin homeostasis. In this new effort the research team has found that it also plays a crucial role in the development of the immune system—specifically, in the development of lymph nodes and Peyer's patches.
Lymph nodes are organs situated throughout the human body, most notably in the armpits. They are a garrison of several types of immunity cells—they serve as a form of net or trap for foreign elements that could potentially cause harm. Peyer's patches are structures similar to lymph nodes that exist in the intestine and serve much the same role in immunity.
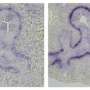
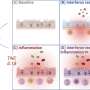
To find out whether a lack of vitamin A during pregnancy might have an impact on immunity in offspring later in life, the researchers fed pregnant mice a diet with little to no vitamin A and then tracked the development of the offspring as compared to the offspring of mice fed normal amounts of vitamin A. The researchers report that the vitamin A deprived offspring developed smaller lymph nodes and Peyer's patches than the control group, and as a result were more susceptible later in life to a virus that causes lung infections—it was introduced intentionally to demonstrate immune response.
The researchers also noted that giving the newly born vitamin A deprived mice the vitamin didn't reverse the impact of the in vitro deficiency, nor did giving them a bone marrow transplant. The smaller lymph nodes and Peyer's patches remained smaller than normal throughout the entire life of the mice contributing to a weaker than normal immune system.
More information: Maternal retinoids control type 3 innate lymphoid cells and set the offspring immunity, Nature (2014) DOI: 10.1038/nature13158
Abstract
The impact of nutritional status during fetal life on the overall health of adults has been recognized; however, dietary effects on the developing immune system are largely unknown. Development of secondary lymphoid organs occurs during embryogenesis and is considered to be developmentally programmed. Secondary lymphoid organ formation depends on a subset of type 3 innate lymphoid cells (ILC3) named lymphoid tissue inducer (LTi) cells. Here we show that mouse fetal ILC3s are controlled by cell-autonomous retinoic acid (RA) signalling in utero, which pre-sets the immune fitness in adulthood. We found that embryonic lymphoid organs contain ILC progenitors that differentiate locally into mature LTi cells. Local LTi cell differentiation was controlled by maternal retinoid intake and fetal RA signalling acting in a haematopoietic cell-autonomous manner. RA controlled LTi cell maturation upstream of the transcription factor RORγt. Accordingly, enforced expression of Rorgt restored maturation of LTi cells with impaired RA signalling, whereas RA receptors directly regulated the Rorgt locus. Finally, we established that maternal levels of dietary retinoids control the size of secondary lymphoid organs and the efficiency of immune responses in the adult offspring. Our results reveal a molecular link between maternal nutrients and the formation of immune structures required for resistance to infection in the offspring.
© 2014 Medical Xpress