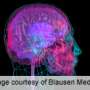
Deep brain stimulation for obsessive-compulsive disorder releases dopamine in the brain
Some have characterized dopamine as the elixir of pleasure because so many rewarding stimuli - food, drugs, sex, exercise - trigger its release in the brain. However, more than a decade of research indicates that when drug use becomes compulsive, the related dopamine release becomes deficient in the striatum, a brain region that is involved in reward and behavioral control.
New research now published in Biological Psychiatry from the Academic Medical Center in Amsterdam suggests that dopamine release is increased in obsessive-compulsive disorder (OCD) and may be normalized by the therapeutic application of deep brain stimulation (DBS).
To conduct the study, the authors recruited clinically stable outpatients with OCD who had been receiving DBS therapy for greater than one year. The patients then underwent three single photon emission computerized tomography (SPECT) imaging scans to measure dopamine availability in the brain.
In order to evaluate the effect of DBS, these scans were conducted during chronic DBS, 8 days after DBS had been discontinued, and then after DBS was resumed. Designing the study in this manner also allowed the researchers to measure the relationship between dopamine availability and symptoms.
During the chronic DBS phase, patients showed increased striatal dopamine release compared to healthy volunteers. When DBS was turned off, patients showed worsening of symptoms and reduced dopamine release, which was reversed within one hour by the resumption of DBS. This observation suggests that enhancing striatal dopamine signaling may have some therapeutic effects for treatment-resistant symptoms of OCD.
First author Dr. Martijn Figee further explained, "DBS of the nucleus accumbens decreased central dopamine D2 receptor binding potential indicative of DBS-induced dopamine release. As dopamine is important for reward-motivated behaviors, these changes may explain why DBS is able to restore healthy behavior in patients suffering from OCD, but potentially other disorders involving compulsive behaviors, such as eating disorders or addiction."
The patients selected for participation in this study had previously been non-responsive to traditional pharmacological therapies that target the dopamine system. These findings suggest that the effectiveness of DBS for OCD may be related to its ability to compensate for an underlying dysfunction of the dopaminergic system. The DBS-related stimulatory increase in dopamine appears to aid patients by improving their control over obsessive-compulsive behaviors.
"It is exciting to see circuit-based DBS linked to molecular brain imaging. This is a strategy that may shed light into the mechanisms through which this treatment can produce positive clinical change," said Dr. John Krystal, Editor of Biological Psychiatry.
He also noted, "It would be interesting to know whether the patients who do respond to dopamine-blocking antipsychotic medications commonly prescribed for OCD symptoms have a different underlying disturbance in dopamine function than the patients enrolled in this study who failed to respond to these medications. Nonetheless, the findings of this study raise the possibility that some deficits in dopamine signaling in the brain that might be targeted by novel treatments may prevent adequate response to conventional treatments for this disorder."
More information: "Deep Brain Stimulation Induces Striatal Dopamine Release in Obsessive-Compulsive Disorder" by Martijn Figee, Pelle de Koning, Sanne Klaassen, Nienke Vulink, Mariska Mantione, Pepijn van den Munckhof, Richard Schuurman, Guido van Wingen, Thérèse van Amelsvoort, Jan Booij, Damiaan Denys (DOI: 10.1016/j.biopsych.2013.06.021). The article appears in Biological Psychiatry, Volume 75, Issue 8 (April 15, 2014), published by Elsevier.