Eye cancer and the relevance of genetic testing
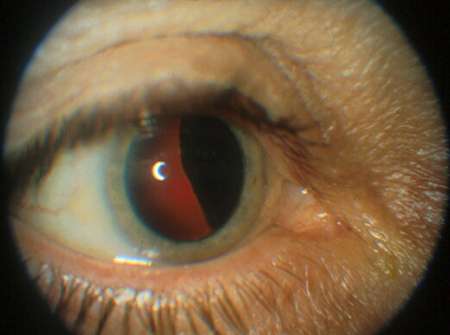
Today is National Eye Patch Day, a fundraising initiative organised by the charity OcuMel UK to increase awareness of a rare eye cancer called 'uveal melanoma' (UM). This is the most common intraocular tumour in adults and about 800 new patients are diagnosed each year in the UK.
Despite successful local control of the eye tumour through eye-sparing radiotherapy or surgery, about half of UM patients develop metastatic disease, which occurs mainly in the liver.
Usually fatal
At present, metastatic UM is usually fatal, as the tumour cells are resistant to current treatment strategies.
A common policy worldwide is to screen all UM patients for metastasis by performing costly six-monthly liver scanning – often using low-resolution tools – and biochemical liver function tests, that are known to be non-specific and often only raised when the secondary disease is very advanced.
In Liverpool, our research group (www.loorg.org), together with the world-leading Liverpool Ocular Oncology Centre, has developed a neural network system that allows personalised prognostication by integrating clinical, histopathological and genetic data from the primary tumour, as well as age and gender of the patient. This service has been in place for several years, has been validated on large data sets, and has been well-received in peer-reviewed scientific journals. It is also popular with the patients.
But why do prognostication testing in UM if the prognosis is so grim?
Through the above prognostication model, UM patients can be stratified with high accuracy into those with 'low' and 'high' risk of developing metastases. Those patients with a low risk of developing secondary disease are referred back to their local eye doctor with reasonable confidence that they will not suffer any further complications from their disease.
Secondary tumours
On the other hand, those UM patients with a 'high' risk tumour are referred to specialist oncologists who perform regular liver screening using high-resolution techniques, with the aim of detecting the secondary tumours earlier. These can be removed using surgery, leading to prolonged survival; this has been demonstrated by researchers in both Liverpool and Paris. When the secondary tumours are not able to be removed surgically, the patients are informed about ongoing clinical trials, investigating promising new medications that are directed to particular targets of the tumour cells.
Eye melanoma is very different to skin melanoma, and is often the 'forgotten cousin'. Through participation in national 'Eye Patch Day', we and the Liverpool clinical team want to help raise awareness of UM, which can affect anyone, and to raise funds, to further advance research with the aim of better understanding this disease and improving patient survival.














