Precision-guided epidurals and better blood monitors
The march of modern medicine is often driven by revolutions in medical imaging. When technology advances, doctors are better able to peer deeply into human tissues, and thus able to detect, diagnose and treat human diseases more effectively.
Now, researchers have taken an established imaging technology called "optical coherence tomography," or OCT, and integrated it with other instruments to bring about the next revolution in imaging by helping doctors provide safer, less painful and more effective care for women in labor and people with diabetic retinopathy and glaucoma. Their research will be presented at CLEO: 2014 being held June 8-13 in San Jose, California, USA.
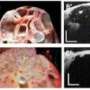
OCT uses scattered "echoes" or reflections of light waves to produce high-resolution images of biological tissues, similar to ultrasound imaging but with one order of magnitude improvement in the resolution. Ophthalmologists have been using OCT to examine the retina for years. More recently, OCT has been applied to a number of other clinical specialties, including oncology for early cancer detection and staging in the gastrointestinal and urogenital tract as well as in cardiology, where it is used to study the formation of plaques in coronary arteries in situ.
Precision-guided epidurals
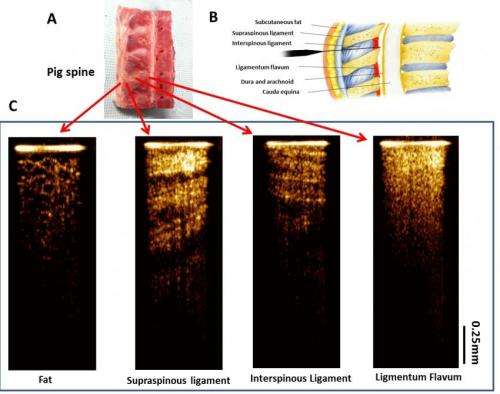
Bioengineer Yu Chen of the University of Maryland and his colleagues have developed a way to integrate an OCT device with an 18-gauge epidural needle. Epidural administration, Chen notes, is traditionally done blindly, using anatomical landmarks. But the team's newly miniaturized handheld device lets anesthesiologists see tissue from the perspective of the tip of the epidural needle, which could help doctors to deliver spinal anesthetic to patients with less pain and fewer complications.
"Due to lack of visual feedback, failure rates are often high, leading to multiple needle insertions," he says. Side effects of these failures can include trauma to blood vessels and punctures in the dura, the outermost membrane surrounding the brain and spinal cord.
"An OCT forward-imaging probe can provide anesthesiologists with real-time visualization of the microarchitecture of tissues and important landmarks, and thus could significantly improve the accuracy and the safety of the needle-based procedure," Chen says.
The researchers have been successful in testing needle-guidance experiments on pig swine samples and hope to conduct a pre-clinical study of the device within the next year.
Presentation AM2O.3, titled "Real-time Epidural Anesthesia Guidance Using Optical Coherence Tomography Needle Probe will take place Monday, June 9, at 11:15 a.m. in Salon V & VI of the San Jose Convention Marriott.
Better blood monitors
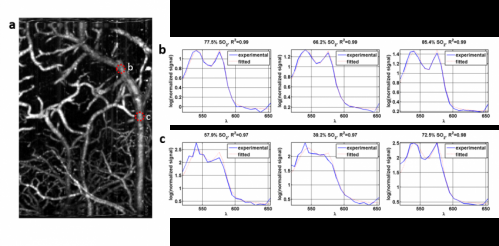
A team at the University of California, Davis, led by Biomedical Engineer Vivek Srinivasan has shown how OCT can simultaneously measure blood flow and blood oxygenation in vessels, without the need for contrast agents.
Like ultrasound, OCT can provide structural information, but it can also be used to determine flow rates and for angiography, visualizing the interior of blood vessels, says Shau Poh Chong, a postdoctoral researcher in the Srinivasan lab.
"Conventional pulse oximetry measures oxygen saturation using transmitted light," Chong says. "Performing these measurements quantitatively with reflected light has traditionally been difficult due to the unknown distance traveled by the light through scattering tissue."
OCT directly determines the distance that light travels. Until now, however, it was difficult to use OCT to measure oxygen saturation in blood, due to additional modeling errors introduced by light scattering. At visible wavelengths, scattering is much lower relative to blood absorption than at infrared wavelengths, where OCT is typically performed. The OCT system developed in the Srinivasan lab uses broadband visible light to measure the amounts of both oxygenated and deoxygenated hemoglobin, the oxygen-carrying protein of blood, thus revealing oxygen saturation levels. In addition, the team developed new methods to further reduce modeling errors caused by light scattering.
"The broad set of measurements provided by the system, including angiography, oximetry and red blood cell flow rates enables the direct assessment of tissue oxygen metabolism, which is essential for understanding the evolution of oxygen supply and demand in numerous disease models," Chong says. "In the future, these techniques could be applied to study metabolic changes in diseases that affect the human retina, such as diabetic retinopathy and glaucoma."
More information: Presentation ATh1O.2, titled "Optical Coherence Imaging of Microvascular Oxygenation and Hemodynamics will take place Thursday, June 12, at 8:30 a.m. in Willow Glen I - III of the San Jose Convention Marriott.