Tailoring treatment in ovarian cancer
(Medical Xpress)—The prognosis for ovarian cancer patients is poor with only 3 out of 10 women living at least 5 years after diagnosis. Clinicians urgently need the tools to provide a more accurate prognosis for patients in terms of whether particular chemotherapeutic agents will be of benefit in their treatment.
UCD researchers led by Dr Amanda McCann have now identified the protein MAD2 as a potential prognostic marker in a number of histological subtypes of ovarian cancer. This may help provide more tailored approaches to the treatment of ovarian cancer patients.
MAD2 is one of the protein components of the spindle assembly checkpoint (SAC) present in all eukaryotes that prevents chromosomes from segregating incorrectly during cell division.
Paclitaxel (Taxol) is the first-line chemotherapeutic agent used to treat ovarian cancer in combination with platinum agents. It works by interfering with the spindle microtubule dynamics to cause cell cycle arrest and cell death (apoptosis), a function mediated by MAD2.
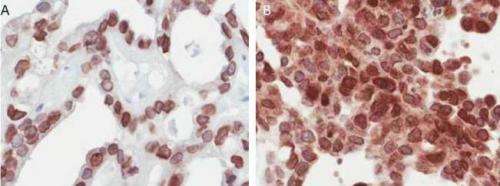
"In this study, we were able to show that low MAD2 nuclear expression associates with a poorer response to chemotherapy and this was exemplified by a shorter time to recurrence of the disease in the patient cohort whose cancer subtype included serous, endometrioid and mixed histologies", explained Barbara McGrogan, the lead author and doctoral candidate in the McCann group.
Serous and endometrioid tumours are biologically different, however, in clinical practice they are still treated similarly. Dr McCann said, "The fact that decreased MAD2 nuclear expression identifies those women with a shorter recurrence free survival irrespective of histological subtype and could help guide clinicians as to whether chemotherapy will actually benefit the patient."
More information: McGrogan B, Phelan S, Fitpatrick P, Maguire A, Prencipe M, Brennan D, Doyle E, O'Grady A, Kay E, Furlong F, McCann A. Spindle assembly checkpoint protein expression correlates with cellular proliferation and shorter time to recurrence in ovarian cancer. Hum Pathol. 2014 Mar 27. pii: S0046-8177(14)00121-X. DOI: 10.1016/j.humpath.2014.03.004. [Epub ahead of print] PubMed PMID: 24792619.