Congenital heart disease specialists develop nonsurgical technique to correct birth defects
A new technique for repairing the most common cardiac birth defect in newborns, commonly referred to as "a hole in the heart," has been used successfully to mend the condition in six premature infants without subjecting the tiny patients to open-heart surgery.
The technique for repairing the condition, patent ductus arteriosus, also called PDA, was published online by the peer-reviewed medical journal Catheterization and Cardiovascular Interventions, the official journal of The Society for Cardiovascular Angiography and Interventions. The study, published in the journal's July print edition, was developed by a team in the Cedars-Sinai Heart Institute's Guerin Family Congenital Heart Program led by Evan M. Zahn, MD, an expert in congenital heart disease.
"Just a few short years ago, the only treatments available for these babies was an intravenous medication regimen or heart surgery," said Zahn, co-director of the Heart Institute's Guerin Family Congenital Heart Program and a leader in the field of nonsurgical cardiac interventions for pediatric patients. "Yet many of these babies are so fragile that we needed additional treatment options to ensure that these children have a healthy future ahead of them."
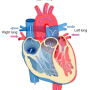
Patent ductus arteriosus is a condition in which a blood vessel called the ductus arteriosus, which routes blood around the baby's lungs prior to birth, does not close naturally as it should within a couple of days after birth. The opening leads to abnormal blood flow and can cause symptoms ranging from fast breathing and difficult feeding to brain hemorrhage and death in premature infants.
The study in Catheterization and Cardiovascular Interventions followed six severely premature infants who were born with patent ductus arteriosus when they were between 26 and 31 weeks gestation. The babies in the study were between 16 and 80 days old and weighed between 1.9 and 4.9 pounds. All the infants in the study had successful closure procedures and did not experience complications.
Zahn and his team – including Alistair Phillips, MD, co-director of the Guerin Family Congenital Heart Program, Ruchira Garg, MD, and Charles F. Simmons, MD, director of Cedars-Sinai's Pediatrics Department and Division of Neonatology and the Ruth and Harry Roman chair in Neonatology in Honor of Larry Baum—developed a catheter-based technique that employed sophisticated imaging technologies fluoroscopy and echocardiography to guide the physicians through the delicate closure procedure.
"The development of new minimally invasive techniques to treat babies with PDA is a major step forward," said Eduardo Marbán, MD, PhD, director of the Cedars-Sinai Heart Institute. "The tiny size of premature infants renders open-chest surgery exceedingly risky; Zahn and colleagues can now fix the problem with a catheter, at the bedside in the neonatal unit, without exposing the internal organs. Lives have been saved, and many others stand to benefit as this new technology is disseminated."