Protein therapy successful in treating injured lung cells
Cardiovascular researchers at The Ohio State University Wexner Medical Center have successfully used a protein known as MG53 to treat acute and chronic lung cell injury. Additionally, application of this protein proved to prevent lung cell injury. Results from this animal model study were just published in the journal Nature Communications.
Jianjie Ma, a professor and researcher in Ohio State's Department of Surgery and the Dorothy M. Davis Heart & Lung Research Institute, first identified MG53 in 2008. In earlier studies, his team showed that MG53 repairs and protects heart and skeletal muscle cells.
"This latest study demonstrates that MG53 is expressed in the lungs and may be used to repair many types of lung injuries," Ma said.
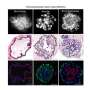
Control animals that lacked MG53 were more susceptible to injury caused by over-ventilation or re-oxygenation when the blood supply returns following a lack of oxygen. In animals treated with recombinant human MG53 (rhMG53), lung cells were protected from injury.
The treatment was given both intravenously and by inhalation. Both delivery methods of the protein therapy reduced symptoms of acute lung injury and chronic emphysema when compared with control animals. Repeated doses improved lung structure in the animals with chronic lung injury. Additionally, researchers noted significant reduction in edema, hypoxemia and inflammatory markers.
"We need to do further testing, but so far this therapy appears safe," Ma said. "The human body already makes small amounts of MG53 in blood circulation, so there is no concern for allergic response. Additionally, we treated rodent models with a dose 10 times higher than the effective dose with no adverse effects."
Acute lung injury can occur in critically ill patients where mechanical ventilation, reperfusion, sepsis, trauma and shock can all lead to lung damage. If the cells cannot repair themselves, it can develop into respiratory failure.
According to the American Lung Association, approximately 36 million Americans live with chronic lung disease, and could potentially benefit from a protein therapy that targets cell repair.
"If treatment with rhMG53 works in humans, the implications for patient care could be quite significant," Ma said. "It could prevent and repair heart and lung cell damage. It could be used prior to surgeries to prevent damage and promote healing. It could be used in an emergency department, by paramedics or on the battlefield to treat traumatic injuries. We are hopeful as we now work to begin our clinical trials."
According to Peter Mohler, director of Ohio State's Dorothy M. Davis Heart & Lung Research Institute, "This new work from Jianjie's team is an excellent example of the type of high-impact, translational science that can occur when creative scientists, surgeons, and cardiologists work closely together on a clinical problem. In this case, it is truly exciting how a discovery in foundational cell biology can potentially lead to new therapies for patients in the clinic."
More information: "Treatment of acute lung injury by targeting MG53-mediated cell membrane repair." Yanlin Jia,et al. Nature Communications 5, Article number: 4387 DOI: 10.1038/ncomms5387. Received 25 February 2014 Accepted 13 June 2014 Published 18 July 2014