Patient stem cells used to make dementia-in-a-dish; help identify new treatment strategy
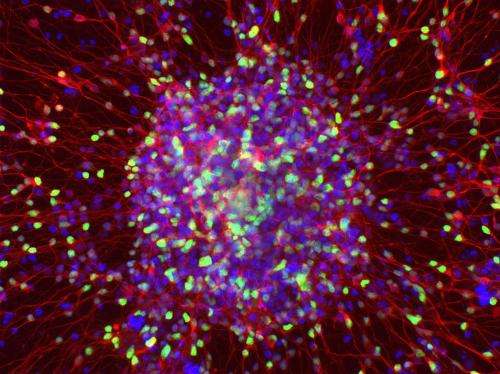
Belgian researchers have identified a new strategy for treating an inherited form of dementia after attempting to turn stem cells derived from patients into the neurons most affected by the disease. In patient-derived stem cells carrying a mutation predisposing them to frontotemporal dementia, which accounts for about half of dementia cases before the age of 60, the scientists found a targetable defect that prevents normal neurodevelopment. These stem cells partially return to normal when the defect is corrected.
The study appears in the December 31st issue of Stem Cell Reports.
"Use of induced pluripotent stem cell (iPSC) technology"—which involves taking skin cells from patients and reprogramming them into embryonic-like stem cells capable of turning into other specific cell types relevant for studying a particular disease—"makes it possible to model dementias that affect people later in life," says senior study author Catherine Verfaillie of KU Leuven.
Frontotemporal disorders are the result of damage to neurons in parts of the brain called the frontal and temporal lobes, gradually leading to behavioral symptoms or language and emotional disorders. Mutations in a gene called progranulin (GRN) are commonly associated with frontotemporal dementia, but GRN mutations in mice do not mimic all the features of the human disorder, which has limited progress in the development of effective treatments.
"iPSC models can now be used to better understand dementia, and in particular frontotemporal dementia, and might lead to the development of drugs that can curtail or slow down the degeneration of cortical neurons," Verfaillie says.
Verfaillie and Philip Van Damme of the Leuven Research Institute for Neuroscience and Disease explore this approach in the Stem Cell Reports study by creating iPSCs from three patients carrying a GRN mutation. These immature cells were impaired at turning into mature, specialized cells called cortical neurons—the most affected cell type in frontotemporal dementia.
One of the top defective pathways in the iPSCs was the Wnt signaling pathway, which plays an important role in neuronal development. However, genetic correction or treatment with a compound that inhibits the Wnt signaling pathway restored the ability of the iPSCs to turn into cortical neurons. Taken together, the findings demonstrate that the GRN mutation causes the defect in cortical neuron formation by altering the Wnt signaling pathway.
"Our findings suggest that signaling events required for neurodevelopment may also play major roles in neurodegeneration," Van Damme says. "Targeting such pathways, as for instance the Wnt pathway presented in this study, may result in the creation of novel therapeutic approaches for frontotemporal dementia."
The researchers will now work to better understand what goes wrong in GRN-mutated cells, as well as identify precise molecular targets that could then be used for drug screens.
More information: Raitano et al. Restoration of Progranulin Expression Rescues Cortical Neuron Generation in an Induced Pluripotent Stem Cell Model of Frontotemporal Dementia, Stem Cell Reports, www.cell.com/stem-cell-reports … 2213-6711(14)00358-0