Heart bypass surgery outperforms new generation stents
Despite the advent of a new generation of stents, patients with multiple narrowed arteries in the heart who received coronary artery bypass grafting fared better than those whose arteries were opened with balloon angioplasty and stents in a study presented at the American College of Cardiology's 64th Annual Scientific Session.
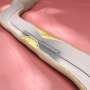
The findings echo past studies, which have shown patients with multiple narrowed arteries have better outcomes with coronary artery bypass grafting, also known as CABG or heart bypass surgery, than with angioplasty, also known as percutaneous coronary intervention or PCI, a less-invasive option in which a stent is inserted to hold the arteries open.
In the new study, patients receiving angioplasty with the new stents had a 47 percent higher risk of one of the outcomes identified as a primary endpoint in the study: death, heart attack and subsequent procedure to clear blocked arteries, as compared to patients who received bypass. In bypass surgery, a vein or artery from elsewhere in the body is grafted onto a narrowed coronary artery to allow blood to flow to the heart more freely. The study reinforces current guidelines, which recommend bypass surgery for treating patients with substantial narrowing in multiple arteries, a condition known as multivessel coronary artery disease.
"Based on our data, CABG is still the preferred option for multivessel disease," said Seung-Jung Park, M.D., a cardiologist at Asan Medical Center in Seoul, South Korea, and the study's lead author. "We had thought that previous trials may have been limited by their use of first-generation drug-eluting stents, but these results show CABG still leads to better outcomes."
The study, called the Bypass Surgery Versus Everolimus-Eluting Stent Implantation for Multivessel Coronary Artery Disease (BEST) trial, is one of only two randomized controlled trials to compare bypass to angioplasty since the introduction of everolimus-eluting stents, a new generation of drug-eluting stent. These stents emit medication to prevent blood clots and have been shown to be more effective at keeping arteries open. The trial's findings align with those from the previous study, called Synergy between PCI with Taxus and Cardiac Surgery (SYNTAX).
The study included 880 patients treated at 27 hospitals in four countries. All patients had multivessel coronary artery disease and were determined to be equally appropriate candidates for either angioplasty or bypass. Half of the patients were randomly assigned to receive angioplasty with everolimus-eluting stent and half received bypass surgery. Patients were tracked for an average of more than 4.5 years.
"During this relatively long-term follow-up, angioplasty was associated with a significant increase in the incidence of the death, myocardial infarction and target vessel revascularization, a difference that was mainly attributed to the higher rate of target-vessel revascularization in the angioplasty group," Park said.
Death, heart attack or a subsequent procedure to clear blocked arteries occurred in 15 percent of patients in the angioplasty group and 11 percent of patients in the bypass group. In addition, the researchers found patients receiving angioplasty were twice as likely to need repeat revascularization and more than 1.8 times as likely to have a heart attack as patients who received bypass.
The study was terminated earlier than planned, limiting its statistical power to detect differences in individual outcomes instead of only composite outcomes. The early termination was due to slow enrollment, thought to be a consequence of the rapid spread and increased appeal of a new angioplasty technique called fractional flow reserve during the later part of the study enrollment period.
The angioplasty procedures in the BEST and SYNTAX studies were guided by the medical imaging technique angiography. Fractional flow reserve, by contrast, allows surgeons to more precisely assess the condition of the arteries based on the pressure of blood as it flows through them and has been associated with better outcomes for angioplasty. A new study is currently underway to compare outcomes from bypass to angioplasty using fractional flow reserve in patients with multivessel coronary artery disease.
Because it is a more invasive procedure, heart bypass is generally recommended only for patients with higher-risk narrowing in two or more arteries. Angioplasty is preferred for patients with lower-risk narrowing in one or two arteries.
More information: This study was simultaneously published online in the New England Journal of Medicine at the time of presentation.