Researchers recommend weight-loss interventions focused on hunger-reducing food choices

A new study suggests that weight-loss interventions that center on hunger-reducing food choices and behavioral support can produce favorable shifts in "self-reward" areas of the brain. The study addresses concerns by weight-loss experts that when instant gratification, or addictive-type food involvement, becomes entrenched in the brain, it may be nearly impossible to reverse.
The study volunteers were 13 overweight or obese men and women assigned to one of two study groups. One group was placed on an at-home weight-loss intervention of lower calorie foods for 6 months with a goal of losing about 1 to 2 pounds per week. The other was a no-intervention control group eating normally at home.
To satisfy brain areas linked with cravings—the intervention group's diet provided about 45 to 50 percent of daily calories from "slow-digesting" carbohydrates and high-fiber foods. High-protein foods and healthy fats each provided about 25 percent of the other daily calories. The group received 1-hour support sessions most weeks and meal plans that centered on hunger reduction, portion-control, and high satisfaction. They were told to evenly space meals and snacks, and to freely use foods from a list of those with very few calories that could be eaten any time. These tips were designed to keep blood sugar levels even (versus spiking) and control hunger.
The study was conducted by senior coauthor Susan B. Roberts—an expert in developing programs for weight management—and colleagues. Roberts is with the Jean Mayer USDA Human Nutrition Research Center on Aging (HNRCA) at Tufts University in Boston. The center is funded by USDA's Agricultural Research Service. She is also professor of both nutrition and psychiatry at Tufts University.
Roberts has centered her work on "innate nutritional neurobiology," which is about helping people learn what "pushes their buttons" when it comes to staying in control of what they eat. "The abundance of affordable commercial foods that contain added sugars and low-satiety, refined grains and starches are food cues that stimulate the American palate," says Roberts. "Our studies have shown that just viewing pictures from mouth-watering food advertisements can activate brain-reward pathways and trigger the urge to eat." By understanding how brain circuitry stimulates eating in response to visual and actual food cues, Roberts has linked reducing cravings and increasing satisfaction with successful weight-control programs.
For the study, the team used magnetic resonance imaging (MRI) to assess neuronal activity in the brain's reward-response areas. The findings indicate that it is possible to change the cycle of constantly craving unhealthy foods by retraining the brain to stop activating its reward centers on exposure to a steady stream of high-calorie food cues. (See sidebar below.) "A particular challenge is ongoing exposure to commercial foods that are formulated to overactivate the brain and trigger constant cravings," Roberts says.
All volunteers had two MRI brain scans—one at the beginning and one at the end of the 6-month study. During scanning, the volunteers were shown 20 images of high-calorie foods and 20 images of low-calorie foods. They rated the desirability of each image on a scale of 1 (none) to 4 (extremely) while blood flow to key brain areas was measured. Higher blood flow indicated greater neuronal activity.
Roberts was not surprised that the intervention group achieved significant weight loss—about 14 pounds. "Our key finding is that intervention-group participants had greater neuronal activity on their brain scans when viewing low-calorie food images at the end of the 6-month period versus when they viewed the same images before the intervention—a significant favorable shift," she says. "More studies to assess whether these positive changes in neuroplasticity can help people sustain weight loss over time are needed."
Strategies To Control Cravings Are Key
Susan B. Roberts has been studying complex brain responses to the dramatically changed U.S. food supply that is described as the "obesogenic environment" in the "Dietary Guidelines for Americans" (DGAs) 2010. Roberts is the director of the Energy Metabolism Laboratory at HNRCA in Boston, which is funded in part by USDA's Agricultural Research Service.
The DGAs report that during the past four decades, the amount of food on hand to purchase from the U.S. market—in terms of average daily caloric availability—has increased by 600 calories per person.
Roberts emphasizes a moderately low carbohydrate intake rather than a very low carb intake, in keeping with the Recommended Dietary Allowance (RDA) for carbohydrates of 130 grams, or 520 calories, per day. "Carbohydrate intake at the lower end of the recommended range, rather than below it, is optimal for weight control," says Roberts. "It is a good level where people can enjoy some carbs, but not so many that they trigger food cravings and eating-control issues."
Another key to managing body weight is getting ample food fiber, which is a subset of the carbohydrate group, says Roberts. The daily adequate intake for fiber is 25 grams for women and 38 grams for men. Unfortunately, dietary fiber intake among U.S. consumers averages only 16 grams per day, according to ARS data from the Food Surveys Research Group in Beltsville, Maryland.
"For losing weight, I recommend at least 40 grams of fiber per day," says Roberts. "Fiber is one of our weight-control cornerstones because it helps achieve the feeling of fullness after eating."
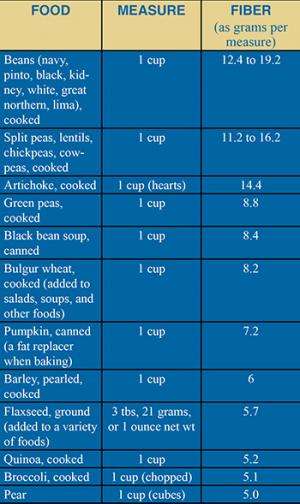
Good sources of fiber include legumes (beans and peas), vegetables, fruits, nuts and seeds, and whole grains. The table below provides a short list of foods that are high in both fiber and slow-digesting carbs.