Demand-driven deep brain stimulation to treat Parkinson's disease
Researchers from the Centre for Biomedical Technology (CTB) at Universidad Politécnica de Madrid (UPM) have participated in a joint research project with Universidad Carlos III de Madrid and University of Reading (United Kingdom) that has revealed possible subtypes of Parkinson's disease patients. By applying this finding, researchers have used artificial intelligence techniques for tremor detection in patients of the discovered groups. The goal is to achieve a demand-driven deep brain stimulation that intelligently alleviates the symptoms of the disease, which would enhance the life quality of patients.
Parkinson's disease is a degenerative disorder of the central nervous system whose main symptomatology includes temblor, rigidity and bradykinesia. The motor function is a balance that is carefully regulated by a set of neurotransmitters in the circuits of the basal ganglia. When a neurotransmitter is not correctly released, the information among cores is inefficient and results in diseases of the motor system. This is the case in Parkinson's disease, mainly caused by the death of dopamine-secreting neurons. The research work of the group of Cognitive and Computational Neuroscience of CTB-UPM is focused on the study of the most commonly known symptom of Parkinson's disease, tremors.
There are diverse types of tremors in Parkinson's disease depending on the circumstances in which it appears. The resting tremor (RT) is the most common symptom. RT is a rhythmic movement that appears when the patient is at rest and usually disappears when the patient starts a movement. This symptom hinders patients from performing daily life tasks.
Diverse studies suggest that Parkinson's disease actually has different subtypes, since not all patients have the same symptomatology or respond in the same way to the treatment.
The treatment of Parkinson's disease is a complex task today. The first choice is oral medication that consists of levodopa (a main precursor of dopamine). Its usage dates to the mid-1960s and it is still the most commonly prescribed treatment. Levodopa therapy alleviates the main symptomatology of Parkinson's disease, but it does not adapt properly to the disease. After a few years using this treatment, normally about five years, patients start to experience motor fluctuations.
This effect is known as the ON-OFF phenomenon, alternate periods in which drugs work (ON) and stop working (OFF). OFF periods increase as this treatment continues. Therefore, oral medication is increasingly inappropriate.
Due to these complications, some patients need surgery in order to be treated with deep brain stimulation. This therapy consists of the implantation of electrodes that apply an electrical stimulation targeted on the affected brain structure, which is usually the subthalamic nucleus in Parkinson's disease. This stimulation inhibits abnormal activity of the neurons, which tend to an excessive synchronization, and imposes a suitable performance.
Although neurostimulators are known as "brain pacemakers," they do not work in the same way. Pacemakers are able to detect atypical episodes of heart signals and adjust the stimulation according to the patients' needs at every moment, while the neurostimulators, once implanted, continuously stimulate the brain. This means that the device battery has to be replaced every three to four years, requiring additional surgery.
The research finds results that, with a high degree of accuracy, give evidence of two subtypes of patients, or more specifically temblor of type 1, according to the Consensus Statement of the Movement Disorder Society on Tremor.
These results can lead to the development of diverse treatments for the different types of patients involved.
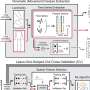
Based on these findings, the study proposes a real-time tremor detection system based on artificial neural networks. Researchers suggest a tool than can learn different characteristics of brain signaling when the patient suffers a tremor. Through training, the device would be able to make a decision regarding tremors. When a demand-driven stimulation system is judged to be 100 percent reliable, it will be embedded in the neurostimulator.
A demand-driven stimulation device would be capable of detecting when the patient is trembling, and only then provide brain stimulation. All this has a double benefit: First, brain structures will be able to work properly when the patients do not show symptoms, rather than being stimulated at all times. Second, batteries would be more efficient, extending the useful life of the device, and consequently, extending the period before surgery for battery replacement.
Researchers hope to provide implantable medical devices with refined artificial intelligence. These devices could learn the pathology of the patient and have the capacity to mtake decisions in order to enhance the treatment and daily lives of patients.
More information: CAMARA, C; ISASI, P; WARWICK, K; RUIZ, V; AZIZ, T; STEIN, J; BAKSTEIN, E. "Resting tremor classification and detection in Parkinson's disease patients". Biomediacal Signal processing and Control, 16 88-97; FEB 2015. DOI: 10.1016/j.bspc.2014.09.006