Mega-doses of Vitamin D may decrease hospital stays for critical care patients, study suggests

Hospitalized patients often have insufficient levels of vitamin D because of the lack of physical activity and exposure to the sun. Vitamin D is thought to increase the ability of immune cells to fight infection.
The 31 patients participating in Emory's randomized clinical trial were divided into three groups. Two of the groups received high doses of vitamin D3 (a total of 250,000 or 500,000 international units over five days), and one received a placebo.
"These dosages were significantly higher than normal daily doses and were intended to quickly restore vitamin D levels in patients who have low levels," says Jenny Han, MD, assistant professor of medicine, Emory University School of Medicine. Han's research career has focused on defining the relationship between vitamin D status and infection.
Study participants who received a placebo had an average blood level of 21 ng/ml vitamin D. The Endocrine Society defines deficiency as less than 20 ng/ml and insufficiency as between 20 and 30 ng/ml.
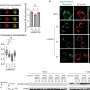
Hospital length of stay went down with the higher dose of vitamin D (average 36 days for placebo, 25 days for lower dose, 18 days for higher dose). This difference was statistically significant.
The length of stay in intensive care also tended to decrease (average 23 days for placebo, 18 days for lower dose vitamin D, 15 days for higher dose vitamin D), but the change was not statistically significant. A similar result was observed for duration of ventilator support.
The majority of the patients in the study had severe sepsis or septic shock; 43 percent had some type of infection upon admission. Some had cardiovascular or neurologic diseases.
According to the study, more research is needed to determine the effect of vitamin D on patient recovery.
"These data can inform the design of a larger, adequately powered randomized controlled trial on the efficacy of high-dose vitamin D3 on host immunity and other indices associated with recovery," the authors conclude.