New treatment approach to limit damage after joint bleed
The results of a study presented today at the European League Against Rheumatism Annual Congress (EULAR 2015) identified that the cytokine (cell signalling protein) Interleukin-1β (IL-1β) is a crucial factor in the development of blood-induced cartilage damage. This finding opens up the possibility that a treatment targeting IL-1β could provide a new way to protect cartilage after a joint bleed, which in turn should significantly reduce subsequent disability.1
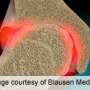
Exposure of joint cartilage to blood can occur after joint trauma, major joint surgery, or due to haemophilia. Joint bleeds, from whatever cause, are expected to lead to an inflammatory response in the joint and to significant destruction of joint cartilage. , Any treatment that could limit the damage resulting from a joint bleed would potentially make a big difference to minimising future disability.
"As therapeutic agents opposing the activity of IL-1β are readily available, further research is now warranted to investigate whether an IL-1β antagonist would be effective in preventing and treating joint damage as a result of bleeding into the joint," said Dr. Simon Mastbergen, principle investigator from the University Medical Centre Utrecht, Netherlands. "Findings also suggest that the quicker treatment is initiated, the less damage to the joint may be sustained," he added.
In contrast, blocking another cytokine - tumour necrosis factor-alpha (TNF-α) - exhibited no effect on blood-induced cartilage damage. "This would appear to rule out TNF-α inhibitors, a class of drug currently used to treat various forms of arthritis, for this new indication," Dr. Mastbergen concluded.
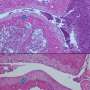
Healthy human cartilage samples were cultured for 4 days in the presence or absence of 50% whole blood. Either IL-1β monoclonal antibody, IL-1 receptor antagonist, or TNF-α monoclonal antibody was added during blood exposure. Subsequent cartilage damage was assessed.
Addition of IL-1β monoclonal antibody or IL-1 receptor antagonist resulted in a dose- and time-dependent protection of cartilage from blood-induced damage, with early administration after blood-exposure found to be the most beneficial. In higher concentrations, almost complete normalisation of cartilage was achieved. In contrast, addition of TNF-α monoclonal antibody exhibited no effect on blood-induced cartilage damage.