Study identifies brain abnormalities in people with schizophrenia
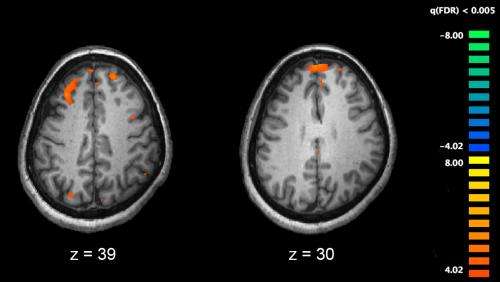
Structural brain abnormalities in patients with schizophrenia, providing insight into how the condition may develop and respond to treatment, have been identified in an internationally collaborative study led by a Georgia State University scientist.
Scientists at more than a dozen locations across the United States and Europe analyzed brain MRI scans from 2,028 schizophrenia patients and 2,540 healthy controls, assessed with standardized methods at 15 centers worldwide. The findings, published in Molecular Psychiatry, help further the understanding of the mental disorder.
The work was the outcome of the Enhancing Neuroimaging Genetics through Meta-Analysis project (ENIGMA), from the Schizophrenia Working Group that is co-chaired by Jessica Turner, associate professor of psychology and neuroscience at Georgia State, and Theo van Erp, assistant research professor in psychiatry at the University of California, Irvine.
"This is the largest structural brain meta-analysis to date in schizophrenia, and specifically, it is not a meta-analysis pulled only from the literature," said Turner. "Investigators dug into their desk drawers, including unpublished data to participate in these analyses. Everyone performed the same analyses using the same statistical models, and we combined the results. We then identified brain regions that differentiated patients from controls and ranked them according to their effect sizes."
The team found individuals with schizophrenia have smaller volume in the hippocampus, amygdala, thalamus, nucleus accumbens and intracranial space than controls, and larger pallidum and ventricle volumes. The study validates collaborative data analyses can be used across brain phenotypes and disorders, and encourages analysis and data-sharing efforts to further understanding of severe mental illness.
The ENIGMA collaborations include working groups for other disorders such as bipolar disorder, attention deficit, major depression, autism and addictions, who are all doing these same analyses.
The next step in this research is to compare the effects across disorders, to identify which brain region is the most affected in which disorder, and to determine the effects of age, medication, environment and symptom profiles across these disorders.
"There's the increased possibility, not just because of the massive datasets, but also because of the collaborative brain power being applied here from around the world, that we will find something real and reliable that will change how we think about these disorders and what we can do about them," Turner said.