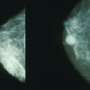
Detecting more small cancers in screening mammography suggests overdiagnosis
Screening mammography was associated with increased diagnosis of small cancers in a study across U.S. counties but not with significant changes in breast cancer deaths or a decreased incidence of larger breast cancers, which researchers suggest may be the result of overdiagnosis, according to an article published online by JAMA Internal Medicine.
The goal of screening mammography is to reduce breast cancer death by detecting and treating cancer early in the course of the disease. If screening detects tumors early, the diagnosis of smaller and more treatable cancers should increase, while the diagnosis of larger and less treatable cancers should decrease. However, there are increasing concerns that screening unintentionally leads to overdiagnosis by identifying small, indolent or regressive tumors that would not otherwise become clinically apparent.
Richard Wilson, D.Phil., of Harvard University, Cambridge, Mass., and coauthors conducted an ecological study of 16 million women ages 40 and older who lived in 547 counties reporting to Surveillance, Epidemiology and End Results cancer registries during the year 2000. Of these women, 53,207 were diagnosed with breast cancer that year and followed up for the next 10 years.
The authors examined the extent of screening in each county and measured breast cancer incidence in 2000 and incidence-based breast cancer death during the 10-year follow-up, with incidence and mortality calculated for each county.
The authors found that across counties there was a correlation between the extent of screening and breast cancer incidence but not with breast cancer mortality. An increase of 10 percentage points in the extent of screening was associated with 16 percent more breast cancer diagnoses but not significant change in breast cancer deaths.
More screening also was associated with increased incidence of small breast cancers of 2 centimeters or less but not with a decreased incidence of larger breast cancers, according to the results. An increase of 10 percentage points in screening was associated with a 25 percent increase in the incidence of small breast cancers and a 7 percent increase in the incidence of larger breast cancers.
"Across U.S. counties, the data show that the extent of screening mammography is indeed associated with an increased incidence of small cancers but not with decreased incidence of larger cancers or significant differences in mortality. ... What explains the observed data? The simplest explanation is widespread overdiagnosis, which increases the incidence of small cancers without changing mortality, and therefore matches every feature of the observed data," the authors conclude.
However, the authors note clinicians are correct to be wary of ecological studies because of ecological fallacy, which is making inferences about individuals from group data in statistical analyses because individuals may not possess those characteristics.
"As is the case with screening in general, the balance of benefits and harms is likely to be most favorable when screening is directed to those at high risk, provided neither too frequently nor too rarely, and sometimes followed by watchful waiting instead of immediate active treatment," the study concludes.
In a related commentary, Joann G. Elmore, M.D., M.P.H., of the University of Washington, Seattle, and Ruth Etzioni, Ph.D., of the Fred Hutchinson Cancer Research Center, Seattle, write: "However, much has also been written about the caution needed when interpreting ecological analyses. It is well known, for example, that ecological studies provide no information as to whether the people who were actually exposed to the intervention were the same people who developed the disease, whether the exposure or the onset of disease came first, or whether there are other explanations for the observed association."
"We need clear communication and better tools to help women make informed decisions regarding breast cancer screening mammography. ... Perhaps most important, we need to learn how to communicate with our patients about uncertainty and the limits of our scientific knowledge. In the end, we all need to become comfortable with informing women that we do not know the actual magnitude of overdiagnosis with precision. Part of informed decision making is providing all the information, even our uncertainty," the authors conclude."
More information:
JAMA Intern Med. Published online July 6, 2015. DOI: 10.1001/jamainternmed.2015.3043
JAMA Intern Med. Published online July 6, 2015. DOI: 10.1001/jamainternmed.2015.3056