Cyclosporine does not improve outcomes after PCI
The immunosuppressant drug cyclosporine did not improve clinical outcomes compared to placebo in patients receiving percutaneous coronary intervention (PCI) for the more severe form of heart attack known as ST-segment elevation myocardial infarction (STEMI).
Results of the CIRCUS trial, presented today in a Hot Line session at ESC Congress 2015, and published simultaneously in the New England Journal of Medicine. showed that the drug, administered prior to PCI, had no impact on a composite of all-cause death, hospitalisation for - or worsening of - heart failure, or adverse left ventricular remodelling at one year.
"We were very surprised and disappointed," said lead investigator Michel Ovize, MD, PhD, from Claude Bernard University, in Lyon, France.
"There is substantial experimental evidence that cyclosporine can reduce infarct size and improve cardiac function, and we previously published a small-size phase II trial suggesting that cyclosporine may reduce infarct size in STEMI patients (N Engl J Med. 2008 Jul 31;359(5):473-81). Obviously, the larger phase III CIRCUS study did not confirm this, and the reason for this discrepancy in unclear."
The study included patients with anterior STEMI undergoing PCI within 12 hours of symptom onset and with complete occlusion of the culprit coronary artery.
Patients were randomly assigned to receive a 2.5 mg/kg intravenous bolus injection of cyclosporine (n=395) or matching placebo (n=396) before coronary recanalization.
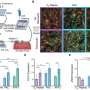
The rate of the primary outcome was 59.0% in the cyclosporine group versus 58.1% in the control group (odds ratio 1.04; P=0.77), and cyclosporine also did not reduce the incidence of separate clinical components of the primary outcome or other events including recurrent infarction, unstable angina or stroke.
"The real-life setting of anterior STEMI is quite different from animal models and, in addition, treatment of patients has changed in several ways since our previous study," said Professor Ovize. "Targeting reperfusion injury to reduce infarct size remains a major challenge for PCI cardiologists in charge of STEMI patients whose cardiovascular risk remains much too high."