Long-term ovarian cancer survival higher than thought
Combing data collected on thousands of California ovarian cancer patients, UC Davis researchers have determined that almost one-third survived at least 10 years after diagnosis.
The unprecedented findings upend the notion that women diagnosed with cancer of the ovary always face a poor chance of survival. In fact, while the study confirmed earlier findings on characteristics associated with ovarian cancer survival—younger age, earlier stage and lower grade tumors at diagnosis—it also identified a surprising number of long-term survivors who didn't meet those criteria.
"The perception that almost all women will die of this disease is not correct," says Rosemary Cress, lead author of the paper, published online today in the Journal of Obstetrics and Gynecology. "This information will be helpful to physicians who first diagnose these patients and the obstetricians/gynecologists who take care of them after they receive treatment from specialists."
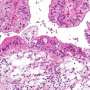
Cress, an epidemiologist and associate adjunct professor in the UC Davis Department of Public Health Sciences, used the California Cancer Registry to analyze data reported on all California residents diagnosed with epithelial ovarian cancer between 1994 and 2001. Epithelial ovarian cancer is the most common type of ovarian cancer, occurring in nine out of 10 cases.
Of the 11,541 patients in the registry database, 3,582 (31 percent) survived more than 10 years, Cress and her colleagues discovered. It was the first time that research has looked at 10-year trajectories for patients; most survival studies have looked only at 5-year survival or less.
As expected, the study found that the majority of the long-term survivors were younger, had early-stage disease when they were diagnosed and their tumors were of a lower-risk tissue type. What struck the researchers was that of the 3,582 long-term survivors, 954 of them had been considered to be at high risk of dying from their disease, either because of their tumor stage, grade or older age at diagnosis.
"This information is important for patient counseling," says study co-author Gary Leiserowitz, a professor of gynecologic oncology and interim chair of the UC Davis Department of Obstetrics and Gynecology. "Many patients and physicians know that ovarian cancer is a dangerous cancer, but they don't realize that there is significant biological variability among patients. It's not a uniformly fatal prognosis."
One such survivor is Jacqueline Price, 74. The Fair Oaks, Calif. woman was diagnosed at age 60 with stage IIIC ovarian cancer. Determined to make the right decision about how to proceed, she asked the doctor for the pathology report.
"It said I had two months and to call hospice," says Price. "I thought, if I only have a couple of months, I want to spend it with my family. I wasn't going to have any treatment. It was doom and gloom."
Leiserowitz, her oncologist, urged Price to reconsider. When the "fog cleared," Price recalls, she opted to go ahead with the surgery, and soon afterward agreed to aggressive chemotherapy treatment.
"I cannot even imagine missing these past 15 years," Price says now. Her experience spurred her to reach out to other ovarian cancer patients and survivors as an advocate and "healing circle" organizer. She says findings from the UC Davis study will help women understand that ovarian cancer is not an automatic death sentence, she says, and empower them to remain optimistic, which in and of itself can benefit survivorship.
Leiserowitz says the next step in the research is to figure out why so many women who are given a poor prognosis eventually beat their odds.
"For a disease that is so dangerous, why are so many surviving?" he asks.
Among the theories, says Leiserowitz, are that ovarian cancer patients who carry mutations in the tumor suppressor genes BRCA 1 and BRCA 2 respond better to chemotherapy than those who don't. He also suggests that other biological differences among patients with advanced ovarian cancer may affect individual outcomes. It's also possible that some patients get more effective treatment than others, boosting their survival odds.
"This is an exploratory study to figure out who has survived," Leiserowitz adds. "We can now go back and look at tumor tissue to do a comparison between long- and short-term survivors to see if there is a genetic basis for that."