New strategy improves detection of genetic mutations in hereditary colorectal cancer
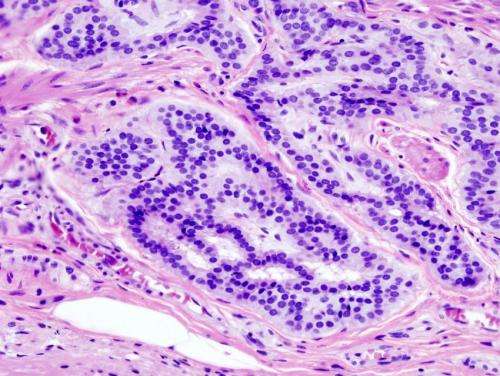
About 3% of colorectal cancers are due to Lynch syndrome, an inherited cancer susceptibility syndrome that predisposes individuals to various cancers. Close blood relatives of patients with Lynch syndrome have a 50% chance of inheritance. The role that PMS2 genetic mutations play in Lynch syndrome has been underestimated in part due to technological limitations. A new study in the Journal of Molecular Diagnostics describes a multi-method strategy to overcome existing technological limitations by more accurately identifying PMS2 gene mutations, which will improve diagnosis and support appropriate genetic counseling and medical management.
The majority of cases of Lynch syndrome are attributed to heterozygous germline mutations in the DNA mismatch repair genes MLH1 and MSH2, and current methods for DNA sequencing and deletion analysis can successfully detect these mutations. However, at least 16% or more cannot be analyzed with these methods because individuals have a mutation in another mismatch repair gene, PMS2 (PMS 1 homolog 2, mismatch repair system component).
Investigators report on a new testing method developed to fill the gap of accurately detecting PMS2 mutations. "PMS2 mutations have been grossly underestimated due to technical difficulties in handling complex genomic structure. A comprehensive approach to unequivocally identify PMS2 mutations remained to be developed," explained lead investigator Lee-Jun C. Wong, PhD, of Baylor Miraca Genetic Laboratory and Department of Molecular and Human Genetics, Baylor College of Medicine (Houston, TX). These issues include the presence of a large number of highly homologous sequences in other genomic regions and the frequent sequence exchange between active and pseudogenes, together with the high frequency of negative staining of PMS2 by immunohistochemistry.
The investigators developed a three-part strategy, combining targeted capture next-generation sequencing (NGS), multiplex ligation-dependent probe amplification, and long-range PCR followed by NGS to simultaneously detect point mutations and copy number changes of the PMS2 gene. "The results from three methods serve as cross validation for enhanced accuracy and reduced turn-around time," commented co-investigator Victor Wei Zhang, MD, PhD, Department of Molecular and Human Genetics, Baylor College of Medicine.
Using this analysis, the researchers identified deletions in the coding region of the gene (in exons E2 to E9, E5 to E9, E8, E10, E14, and E1 to E15), duplications (E11 to E12) on two chromosomes, and a nonsense mutation. "The homozygous duplication involving exons 11 and 12 is a novel finding," noted Dr. Wong. Clinically, this patient with the E11 to E12 duplication had café au lait spots and was diagnosed with uterine cancer at age 27 and colon cancer at age 43.
According to Dr. Wong, "This combined strategy provides us with a new tool for reliable molecular analysis of any genes containing multiple copies of highly homologous sequences and should improve the positive finding rate for patients with Lynch syndrome if the PMS2 gene is suspected to be defective. Unambiguous identification of exon 14 deletion in patients with suspicious Lynch syndrome reflects the main advantage of this approach, since traditional molecular methods cannot distinguish the deletion of the active gene from that of the pseudogene due to frequent gene conversion between these highly homologous sequences."
In January 2009, the Evaluation of Genomic Applications in Practice and Prevention (EGAPP) Working Group issued recommendations regarding genetic testing strategies in patients newly diagnosed with colorectal cancer. Although only 2% to 4% of colorectal cancers are due to Lynch syndrome, identification of these individuals is seen as a critical way to improve their own health as well as the health of their blood relatives, who have a high chance of having inherited the condition. Individuals with Lynch syndrome have a 16% risk of developing a second primary colorectal cancer within 10 years, and first- or second-degree family members with Lynch syndrome face a 35% to 45% risk of a new cancer by age 70. Once diagnosed with Lynch syndrome, individuals who have not developed cancer would be offered regular colonoscopies and other surveillance testing for colorectal, endometrial, or other cancers.
According to the National Cancer Institute, colorectal cancer is the 4th most common cancer in the U.S. and is expected to result in 49,700 deaths in the U.S. in 2015 with 132,700 new cases diagnosed in that year. It is more common in men than women and is most frequently diagnosed in individuals aged 65 to 74 years.
More information: "A Comprehensive Strategy for Accurate Mutation Detection of the Highly Homologous PMS2 Gene," by Jianli Li, Hongzheng Dai, Yanming Feng, Jia Tang, Stella Chen, Xia Tian, Elizabeth Gorman, Eric S. Schmitt, Terah A.A. Hansen, Jing Wang, Sharon E. Plon, Victor Wei Zhang, and Lee-Jun Wong (DOI: dx.doi.org/10.1016/j.jmoldx.2015.04.001). Published in the Journal of Molecular Diagnostics, Volume 17, Issue 5 (September 2015)