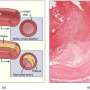
False alarm from the body may be responsible for acute pancreatitis
Researchers at Lund University in Sweden may have discovered one of the keys to understanding how the body develops acute pancreatitis. The results offer hope for the development of drugs that specifically target the disease.
Within gastro research it is a well-known fact that the excessive activation of a type of white blood cells, neutrophils, causes the inflammation of the pancreas. Until now, however, there has been no satisfactory explanation for what causes neutrophil activation. Three research groups at Lund University have worked together to find an answer.
"Our studies show that neutrophils can form web-like structures of DNA and proteins that are harmful to the pancreas. These structures are usually beneficial – they are one of the body's defence mechanisms against infection – but when it comes to pancreatitis, they are activated by something that can be compared to a false alarm, and instead they become destructive", explains Henrik Thorlacius, professor at Lund University and senior physician at Skåne University Hospital, who together with PhD student Mohammed Merza conducted most of the research.
The false alarm is triggered by certain alarm molecules warning for bacteria and viruses that can lead to infections. But acute pancreatitis is a so-called sterile inflammation, and unlike many other inflammations, it is not a response to an infection, which the body is tricked into believing.
During the last 10 years, research about these web-like structures called NETs (Neutrophil Extracellular Traps) has taken off, and the knowledge about their potentially damaging effects has developed. Apart from pancreatitis, this applies to inflammation of the liver and lung, the rheumatic disease SLE, and other inflammatory diseases.
There is currently no drug or treatment that specifically targets pancreatitis; rather, the patient care focuses on life support for heart, lungs and other organs that fail due to this condition. The care, which can be highly unpleasant for the patient, leads to recovery in most cases, but a smaller proportion suffer a fatal outcome.
Henrik Thorlacius has conducted research on the treatment of acute pancreatitis for a long time, and has previously identified several important signalling systems. He considers these new findings to be the most promising so far, and believes that focusing on the NETs and how to make them safe could be a victorious strategy in the search for new treatments.
In the study, mice were injected with bile salt into their pancreas, and then studied throughout the course of the disease. In the complementary part involving human patients, the NETs levels in blood samples from 10 patients suffering from pancreatitis and a healthy control group were studied. The work was facilitated by modern imaging technique using an electron microscope.
More information: "Neutrophil Extracellular Traps Induce Trypsin Activation, Inflammation, and Tissue Damage in Mice with Severe Acute Pancreatitis." Gastroenterology. 2015 Aug 21. pii: S0016-5085(15)01194-4. DOI: 10.1053/j.gastro.2015.08.026