Chemotherapy can cause tumor evolution

Russian scientists have found that neoadjuvant chemotherapy in patients with breast cancer can stimulate evolution of the tumor. The results of the research conducted by Nicholay Litvyakov, D.Sc. at Cancer Research Institute, Head of the Tumor Virology Laboratory, and TSU researcher Marina Ibragimova, were published in Siberian Journal of Oncology.
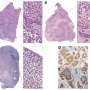
Scientists conducted a study in which they analyzed biopsies of breast cancer patients preparing for operation. In each biopsy, researchers examined the genetic landscape for chromosomal abnormalities.
Before the operation, the women received two to four courses of neoadjuvant chemotherapy (NAC). Repeated analyses were taken after surgery to see the therapy effect on the tumor.
TSU scientists have found that chemotherapy fully or partially destroyed the tumor clones in the majority of patients, but 23 percent of women surveyed showed new tumor formation under the influence of NHT. Some chromosomes or partial chromosomes doubled in these clones, and the tumor cells became more resistant. This phenomenon is called amplification, and is a negative consequence of chemotherapy—almost all of these patients developed metastases, while the remaining patients had no metastases in the five-year period of observation.
The researchers concluded that under the influence of chemotherapy, it is possible to stimulate the evolution of a resistant tumor that does not respond to the effects of chemotherapy.
"We have preliminary results indicating that chemotherapy may cause the appearance of mutations which had not been observed before in the form of amplifications of chromosomal regions. In some cases it was a reason for occurrence of hematogenous metastasis," says Ibragimova. "We should find out the causes and methods for anticipating tumor development. Thus there is no doubt that chemotherapy shall have strictly personalized character, depending on the properties of tumor and patient."
Most chemotherapy drugs are inherently mutagens; chemotherapy may cause genetic disorders in tumor cells. These genetic disorders may lead to illumination or change of tumor cells. Thus, we can observe the occurrence of "clones" of the tumor cells, which are able to cope with the chemotherapy. The researchers are attempting to discover in which cases the tumor may develop under effect of chemotherapy, and how such changes occur.
"That is very interesting observation," says Ibragimova. "Now, we are extending our samples in order to check these observations. If we succeed we would create a technology allowing to predict development of tumor in a specific patient and to define whether this patient needs chemotherapy and which medicines should be prescribed."
The results will help to personalize the treatment process for women with breast cancer. For now, chemotherapy is one of the main tumor treatment instruments for oncologists. Reporting on this topic was held at the plenary session of the 19th Russian Cancer Congress.