Will blocking IL-17A help treat kidney disease?
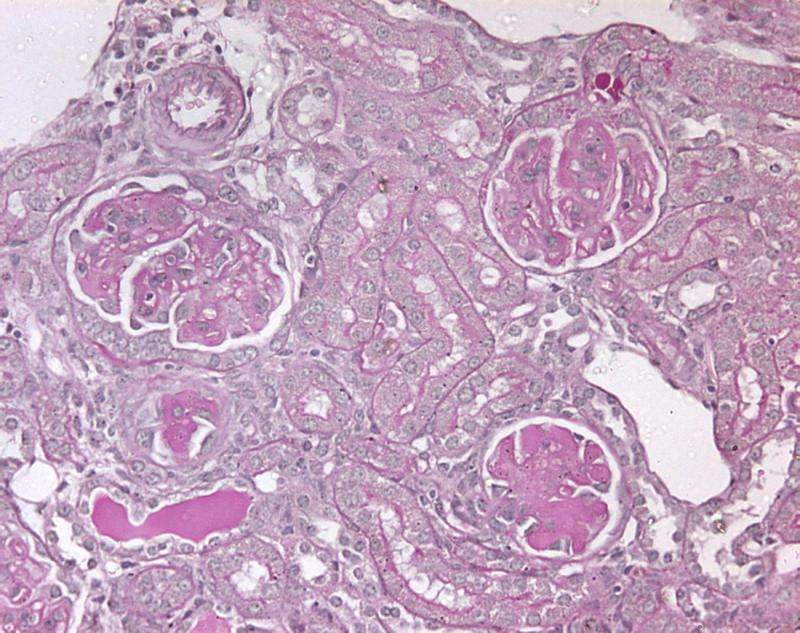
Many different diseases and insults can injure kidneys, resulting in kidney failure. Some autoimmune diseases damage glomeruli (the 'filtering units' of the kidney), while problems with the tubules (for example, impaired blood flow to the kidney at the time of renal transplantation, radio-contrast dye or drugs) can cause acute kidney injury (AKI). A common outcome in either type of injury is that immune cells infiltrate the kidney and this inflammation can result in permanent scarring.
Since the discovery of the proinflammatory cytokines, interleukin (IL)-17A and IL-17F in the early 1990s, many immune cells have proven to be a source of these cytokines, including some T helper cells, now called Th17 cells. Recent human trials of biological therapies targeting IL-17A, components of its receptor or precursor cytokines, have significantly improved clinical disease in some conditions where Th17 cells are implicated—particularly psoriasis.
We have reviewed the research that indicates that IL-17A/F and Th17 cells contribute to renal injury. Animal studies of diseases damaging glomeruli suggest that they are involved in the initial inflammatory response within the kidney. In studies of patients with autoimmune diseases, such as systemic lupus erythematosus, elevated IL-17A levels and higher proportions of Th17 cells in circulating blood have been found, correlating with disease severity. Animal models of AKI have demonstrated that administration of an antibody against IL-17A reduces renal injury. Therefore, blockade of IL-17A/F signaling may be a promising avenue to explore in clinical trials as a novel therapy for the treatment and prevention of immune mediated renal diseases.
More information: Joanna Ghali et al. Targeting IL-17 and IL-23 in Immune Mediated Renal Disease, Current Medicinal Chemistry (2015). DOI: 10.2174/0929867322666151030163022














