February 9, 2016 report
Researchers use genetically modified circulating tumor cells to kill other tumors
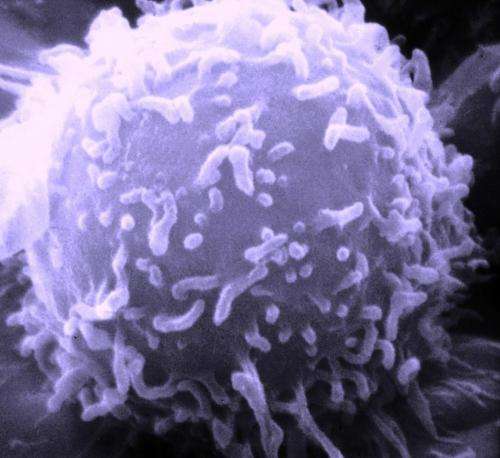
(Medical Xpress)—An international team of medical researchers has found a way to use a kind of cancer cell as a cargo vessel of sorts to kill already existing tumors. In their paper published in Proceedings of the National Academy of Sciences, the group describes how they genetically modified a certain type of cancer cell to kill existing tumors on contact, and the results they found using their approach in test mice.
One of the ways that researchers would like to combat tumors is by injecting a silver-bullet of sorts into the bloodstream that would move about the body until it finds a tumor—when it does, the bullet would open and pummel the tumor with chemicals known to kill tumors. This approach would allow for targeting tumors without harming other parts of the body. Up till now, such research has focused primarily on developing manmade nanoparticle delivery agents—in this new effort the researchers took a whole new approach.
Prior research has shown that the way that cancer spreads is via circulating tumor cells (CTCs)—actual tumor cells that break off from the tumor and travel to other parts of the body though the blood stream—at some point they stop and begin multiplying, causing the growth of new tumors. But other research has shown that CTCs also return to the original tumor (or stop at other tumors) and begin multiplying, making it difficult to completely kill a tumor. It was that second property that was at the center of this new research—the team captured some CTCs from several mice that had three different types of cancerous tumors and then genetically modified the CTCs to express an anticancer cytokine (they liken it to affixing warheads to a missile). Those genetically altered CTCs were then injected back into the mice to see if they would carry the tumor toxin to the existing tumors and then either kill them or slow their growth. The CTCs did find the tumors and when they arrived, they unleashed the tumor toxin, reducing tumor growth by on average 50 to 65 percent in several test mice.
More work will need to be done with this new approach , of course, most specifically to make sure that injecting the modified CTCs will not cause new tumor growth in other parts of the body, and then, to test to see if genetically modified CTCs work the same way in people.
More information: Self-targeting of TNF-releasing cancer cells in preclinical models of primary and metastatic tumors Eleonora Dondossola, DOI: 10.1073/pnas.1525697113 , www.pnas.org/content/early/2016/02/04/1525697113
Abstract
Circulating cancer cells can putatively colonize distant organs to form metastases or to reinfiltrate primary tumors themselves through a process termed "tumor self-seeding." Here we exploit this biological attribute to deliver tumor necrosis factor alpha (TNF), a potent antitumor cytokine, directly to primary and metastatic tumors in a mechanism that we have defined as "tumor self-targeting." For this purpose, we genetically engineered mouse mammary adenocarcinoma (TSA), melanoma (B16-F10), and Lewis lung carcinoma cells to produce and release murine TNF. In a series of intervention trials, systemic administration of TNF-expressing tumor cells was associated with reduced growth of both primary tumors and metastatic colonies in immunocompetent mice. We show that these malignant cells home to tumors, locally release TNF, damage neovascular endothelium, and induce massive cancer cell apoptosis. We also demonstrate that such tumor-cell–mediated delivery avoids or minimizes common side effects often associated with TNF-based therapy, such as acute inflammation and weight loss. Our study provides proof of concept that genetically modified circulating tumor cells may serve as targeted vectors to deliver anticancer agents. In a clinical context, this unique paradigm represents a personalized approach to be translated into applications potentially using patient-derived circulating tumor cells as self-targeted vectors for drug delivery.
© 2016 Medical Xpress